Mia’s story
"Mia wasn’t herself for a while. Sometimes worries about her side hurting, asking what might happen. I reassured her she’d be fine. A couple of times, she got emotional, saying no one knew what she’d been through except me."
Larissa shares her daughter Mia’s acute pancreatitis story with the hopes of raising vital awareness and helping others to get the support that they need.
Tell us a little about yourself
“I’m Larissa from Kent, a single mum to my six-year-old daughter, Mia. She loves school and she’s doing very well. I work with adults with learning disabilities, I’m also a cleaner, and I recently started my own travel business.”
Can you describe when Mia’s symptoms started and what they were?
“In 2023, Mia was four and had been in reception for just a month when I got a call from school. She was crying in pain and kept touching her belly. She had just started on lactulose for her bowels. At first, a check-up at our local hub didn’t show anything, and I was told to give her paracetamol.

A few days later, in the middle of the night, Mia woke up curled in pain, pointing to her chest saying, “It hurts here.” Paracetamol didn’t help, and she kept vomiting, her belly swelling, and she looked pale. I took her straight to A&E. She could barely walk and was being sick. The hospital tried a fluid challenge (giving a small amount of fluid over a short period to assess her body’s ability to tolerate fluids and prevent further dehydration), but she continued to be unwell.”
Talk us through Mia’s journey with acute pancreatitis
“At A&E, they put a cannula in her hand to give fluids. Doctors and nurses asked questions, but didn’t know what was wrong. After 24 hours, Mia was moved to the ward where a cannula was placed in her foot. She had been vomiting all night. The consultant examined her belly and said, “I think this is pancreatitis. We’ll do an ultrasound and maybe an MRI if the ultrasound isn’t clear.”
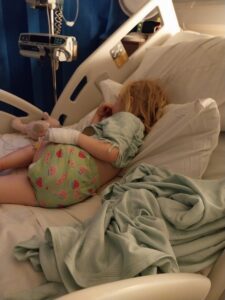
Soon after the tests, she said, “It is pancreatitis, and we need to take her to the high-dependency unit (HDU, specialist wards providing treatment and monitoring for people who are in a critically ill or unstable condition).” In the HDU, Mia had a further cannula inserted in her arm. She had many blood tests and was given medication, including Omeprazole (a medication used to treat heartburn and indigestion), morphine and tramadol for pain relief, and antibiotics. She didn’t eat for about five days and stayed in the HDU for four days.”
What happened afterwards?
“Mia finally left the hospital after two weeks and didn’t return to school for another two weeks. Genetic testing showed she had a single rare CFTR gene mutation that increased her risk of pancreatitis. In the last two years, she has had regular ultrasounds and blood tests. Doctors have explained she could have another attack, as it’s unpredictable, and she may be at risk of developing type 1 diabetes in the future.”
How did this impact you and Mia emotionally?
“Seeing Mia in the hospital was incredibly tough. She was hooked up to heart monitors, and I kept thinking how strong-willed she is and hoping she would make it. I tried to stay strong, but I broke down a few times, wondering how this had happened. For a year, my anxiety was high. I worried about whether her symptoms would return and had to go to the doctors frequently. It traumatised me.

Mia wasn’t herself for a while. She dislikes needles and sometimes worries about her side hurting, asking what might happen. I reassured her she’d be fine. A couple of times, she got emotional, saying no one knew what she’d been through except me. I reminded her that others would understand too. She missed the second month of school but eventually bounced back and regained her confidence. Now she’s thriving at school.”
How did you explain everything that happened to Mia?
“Mia was only four during her acute pancreatitis, so she wasn’t aware of what was happening in HDU. When we went for genetic testing six months later, she asked why. I told her it was to find out why she became unwell and explained a little about genetics in a way she could understand.

Now she’s a bit older and asks lots of questions at the hospital appointments. The medical team explains things to her. At school, Mia wanted to share her experience with her friends. We put up pictures on a tapestry, and she explained what had happened. This helped her process the experience and raised awareness among her classmates.”
How are you and Mia now?
“It’s changed us. I now know what to look out for. Mia still has some severe constipation, and some days she complains of side or back pain. I have to figure out whether it’s constipation or pancreatitis, thinking about where the pain is, how bad it is, and whether she’s had a bowel movement. It’s become part of our daily routine.
Mia eats a normal diet like any other child, and doctors advise just to carry on as usual since pancreatitis can be unpredictable. Each year, she has blood tests, ultrasounds, and stool sample checks to monitor her health.
The first year and a half was tough. Pain and constipation sometimes caused big behaviours, often at school, and staff didn’t always know about pancreatitis. Things have eased over the last six months, and now Mia is happy, healthy, and thriving.”

Would you have any advice for other parents and carers?
“My advice would be to stay as strong as you can, because your child will feel your emotions. Speak to someone you trust and seek professional support if needed, as it can be an emotional time.
Don’t forget to ask questions and get all the information you can. I wish I’d done more of this at the hospital, like asking what was happening next and why. It’s stressful not knowing, so being informed really helps.”
What is one thing you wish people knew about acute pancreatitis?
“I hadn’t heard of acute pancreatitis before Mia was diagnosed. I thought it was a bowel issue because of her lactulose. Children can get acute pancreatitis, and it can be severe. Knowing a little beforehand would have helped me prepare, but it was completely unexpected and frightening to see her so unwell.”
Why would you like to share your story with Guts UK charity?
“I want to help people understand that digestive problems can happen at any age and aren’t talked about enough. Most people shield kids from these things, but children should be able to talk about what has happened to them and express how they feel. Sharing our story could potentially help another family.”
Why are you supporting Guts UK charity today?
“I support Guts UK because raising awareness about digestive conditions is so important. I hope sharing Mia’s story can help others understand these conditions and improve care for families like ours.”
What are your hopes for the future?
“I hope more people are aware that digestive conditions aren’t just adult issues. I want people to understand that even organs you can’t see are vital, just like any other organ we rely on to function properly.”
What you can do to support vital research into pancreatitis

There is no effective treatment for pancreatitis. There is no cure.
Guts UK is dedicated to finding an effective treatment, a cure for this misunderstood and underfunded condition. We are building a community affected by pancreatitis, comforted in knowing they’re not alone.
Our guts have been underfunded and misunderstood for too long. Together, we can change that. For just the price of a cuppa each month, you can regularly donate to our life-saving research today.



