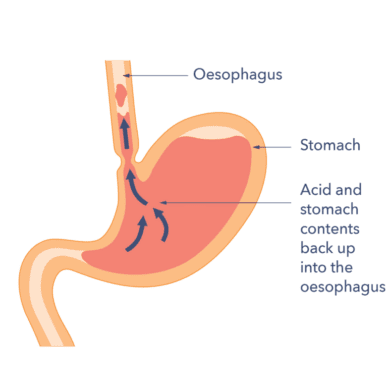
Steven’s story – Oesophageal cancer
In early 2021, Steven's GP told him "this could be nothing, but it could also be cancer." In July 2021, he was diagnosed with stage four oesophageal cancer.
Tell us a little bit about you
“I’m Steven, I’m 50 and I’m married to Laura. I was born in Zimbabwe and moved to the UK in the year 2000 We have three children together, Courtney (26), Michael (24) and Jessica (22). I’ve worked in IT all my life and loved my work.”
When did your symptoms begin?

“In early 2021, I began having difficulty swallowing. I thought maybe I was eating too quickly and food like bread would stick in my throat. By May 2021, it worsened and acute pain whilst swallowing started. My family would worry at the dinner table, waiting to see if I’d be in pain or not. I went to see my GP and he said “This could be nothing, but it could also be cancer”. Cancer had never once crossed our minds. I was in complete shock.”
Talk us through your journey to diagnosis

“I was referred to an Ear, Nose and Throat (ENT) specialist at first who by the end of May, had looked via a camera at my throat and couldn’t see anything. An MRI scan of my neck in June showed no abnormalities. The Barium swallow by the end of June was different. The person who carried out the test was hesitating to tell me something, all he kept saying was, “Don’t worry, we’ll take care of you”.
I was diagnosed in July 2021 with stage four oesophageal cancer. The rollercoaster ride began… Scans, appointments, tests and signing forms (one had nine pages of chemotherapy side effects). There was no time to breathe or absorb new information in between appointments, everything went so fast.”
What was your treatment plan?
“At first, the hospital told me they couldn’t do surgery as the cancer had spread to some lymph nodes in my neck and referred me for palliative therapy. It felt like the end of my life was imminent, we were so emotional. We ended up being referred to another hospital closer to home and the surgeon there said, “Look, it’s in a difficult place, but I’m willing to do the surgery”. Relief washed over us, and I began the pre-operative chemotherapy, which made me incredibly ill.
I had oesophagectomy surgery in early January 2022 and was expected to spend a few weeks recovering in ICU and on the GI ward, but I was out of hospital and heading home after just seven days. I’d been working so hard with the physiotherapy team to recover and get moving. No word of a lie, it felt like I was in the strongest man competition! The staff lined the hospital corridor to wave goodbye to me.
The post-operative chemotherapy began in March 2022, and in-between my first and second session, we discovered that the results from the tumour and margins removed during surgery, showed that I had a complete pathological response to the pre-operative chemotherapy, and there were no viable tumour cells! We were elated. My surgeon called and said the whole room of healthcare professionals cheered. With this news, we decided to do two (instead of four) rounds of post-operative chemotherapy, because we were concerned about just how unwell it was making me. The chemotherapy stopped in May 2022.”
How were you doing at this point?

Throughout, my employers had been so supportive, giving me the time I needed to get better, plus financial, and emotional support. Now, I needed to recover from the chemotherapy and get back to work. I had many complications throughout, including lung issues, which were a direct result of my surgery.
Because of my lungs, I had physiotherapy for my diaphragm, to help me get the most out of my reduced lung capacity. I remember being asked to balance on one foot, and I couldn’t…. and it reminded me of times where I’d be walking with my wife, and I’d bump into her. Sometimes I’d struggle to find words too, but we put it down to “you can’t jump out of bed and run a marathon”. I reminded myself to be patient and kind with myself.
But one morning I woke up barely able to speak or walk. We called the doctor, who told us to, “Go straight to A&E, I’ll call ahead”.
What happened at hospital?

“The cancer had returned. This time, a brain tumour. I had an operation to remove the tumour. I could talk and move well after the operation in September, and the next step was radiotherapy on the brain in October 2022.
We were told it wasn’t unusual to have complications like seizures. My first was sudden and scary. I was having issues with aspirating into my lungs too and getting chest infections. When you have an oesophagectomy, you can’t lie down properly. You have to sleep upright, so contents in your stomach don’t come up and go into the lungs. Thankfully, a brilliant doctor reviewed my PPI medication, and it was a complete game changer! I no longer have to sleep with one eye open.
I had a further small brain tumour in August 2023, and we hopped straight back on the rollercoaster. But by this point, I’d parted ways from my job so I could fully focus on my health.”
How are you now?
“I’m not fully in the clear, but I’m stable. I’m beginning the journey of accepting the new me, and it was sheer determination to survive that got me through this journey.”
What are your hopes for the future?

“Earlier diagnosis of oesophageal cancer is important to me. Looking back, I’d probably had undiagnosed Barrett’s oesophagus as I experienced acid-reflux for 20 years. If I’d been monitored for oesophageal cancer like those with Barrett’s are, it might’ve been found sooner. People need to be diagnosed sooner, so they don’t have to have such life-changing treatment that I’ve had. This is why Guts UK’s research and work is so important.
I share my story today because I was in my 40s when experiencing this. I was relatively young compared to other people in hospital at the time, so had this feeling of being alone. If this story resonates with someone or helps, I will be happy.
The NHS has been amazing. I want to pass on the kindness I’ve received from the people that helped me by sharing my story. A small thank-you for everything that the NHS has done for me.
The statistics weren’t in my favour. To those in despair, I’d like to say that there is always hope. But in order to get a miracle, you first have to believe it can happen to you! And I’ve had three.“
 Guts UK is the only UK charity funding research into the digestive system from top to tail; the gut, liver and pancreas.
Guts UK is the only UK charity funding research into the digestive system from top to tail; the gut, liver and pancreas.
People are suffering. People are dying. All because of a lack of knowledge about our guts. Guts UK exists to change that.
With new knowledge, we will end the pain and suffering for the millions affected by digestive diseases. Please consider donating today. Your donation will help fund research leading to earlier diagnoses, kinder treatments and ultimately, a cure.