Cherylyn’s story – Crohn’s disease
"I don’t feel like I had the same teenage experience as everyone else. The onset of Crohn’s at such a young age was destabilising, and I compared myself to those around me, feeling inferior. I felt that people around me judged me as being different, too."
Note: At Guts UK, we want our stories to be easy for everyone to understand. If any medical terms in Cherylyn’s story are unfamiliar, you can find definitions in our medical glossary at the bottom of this page.
Tell us a little about yourself
“I’m Cherylyn, and I’m 44. I’m the Research Funding Officer here at Guts UK. I live in Barnsley with my husband, Ryan, and our little boy, Oliver. In my spare time, I love jogging, spending time with my loved ones and gardening.”

When did your Crohn’s disease symptoms begin, and what were they?
“When I was around 7 years old, I suddenly lost a lot of weight unintentionally. I remember going for a poo, seeing blood and shouting for my mum. There was another time when I was in town with my mum and suddenly felt faint. Mum took me to the doctors, an ambulance was called, and I was admitted to hospital. I had blood tests, which revealed a blood trait called thalassaemia and severe iron-deficiency anaemia. I just put everything I was feeling down to this.
When I was around 9 years old, I was prescribed iron injections, but nobody investigated the cause of my anaemia. I thankfully put on weight, and my symptoms didn’t become more severe.”

Talk us through your time at secondary school
“When I was 15, the real onset of my Crohn’s disease symptoms started. Again, I lost a lot of weight and had frequent urgency to use the toilet for diarrhoea, as well as mouth ulcers, my hair falling out and feeling lethargic. I dreaded eating and would brace myself for the agonising stomach pain that followed. I started going home from school for my lunch, to use the toilet for diarrhoea, then ended up going back to school pretending to be okay. At my worst, I’d use the toilet over 20 times a day. I experienced stunted growth and delayed puberty, and felt so different to everyone around me.
I remember sitting my GCSEs in agony, with sweat running down my face, and running home afterwards to curl up on the sofa. It was one of the hardest times in my life. Even with all that to contend with, I passed my GCSEs and was so proud of myself.
I started my A-levels and tried to go to college, but had to drop out of both after a few months. My symptoms were relentless. I had lost all my appetite, and someone told me that I looked green. I’d sit in the toilet at school and college with explosive diarrhoea and dread someone hearing me. At home, I remember crawling to the toilet, sobbing my heart out in agony. I felt so alone, and the emotional aspects often felt worse than the physical. I told my mum I couldn’t do it anymore. I just wanted answers.”
Looking back, how does this make you feel about your teenage years?
“I don’t feel like I had the same teenage experience as everyone else. The onset of Crohn’s at such a young age was destabilising, and I compared myself to those around me, feeling inferior. I felt that people around me judged me as being different, too. It was hard not to start puberty until later, not having relationships, and not living that stereotypical teenage life. I was surviving, but on the inside, I felt so lost.”
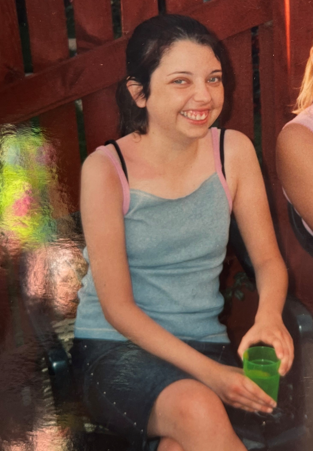
When did you get your Crohn’s disease diagnosis?
“When I was 17, my GP referred me for a colonoscopy, which showed severe Crohn’s disease, mainly affecting my jejunum. My diagnosis made me feel such conflicting emotions: relief that there was a cause and validation that it wasn’t just something I was imagining, but also intense fear for my future.”
What treatment have you received for Crohn’s disease?
“I was prescribed steroids immediately. I felt much better straight away, but had side effects such as hot flushes. My face swelled up, and my appetite came back with a vengeance. The doctors would try to reduce my steroids and try me on a different medication. At this point, I had a different registrar consultant at every appointment. There was no consistency in my care.
I’ve been prescribed so many medications for Crohn’s, including injections and periods where I was put back on steroids. I also was on the elemental diet for nine months. I remember on Christmas Day sipping a supplement drink whilst everyone else was tucking into their Christmas Dinner. Every day felt like the same, and I couldn’t work for several years.”
What happened when you were in your early twenties?
“Around the age of 24, I met a new consultant. He changed my life for the better. He managed to get NHS funding approved to put me on a new treatment called Infliximab. This worked well until my treatment cycle got messed up and I went into a flare-up again. When I was 26, I was put on adalimumab, which was a game-changer for me. To start with, the regime of going to the hospital to receive the treatment was hard, then I learnt to self-inject at home every two weeks.”
How are you now?
“Ever since then, I get put back on adalimumab when I have a flare-up. I take an immunosuppressant called mercaptopurine every day. My last significant flare-up was in 2015. I feel incredibly grateful to have been in remission for so long. I still experience fatigue and irritable bowel syndrome (IBS), which mimics my Crohn’s symptoms to a lesser extent. I have an amazing hospital team, and I have regular blood tests quarterly. I also have a colonoscopy every three years due to my increased risk of bowel cancer.
Last year, I had my symptoms investigated when I thought I was flaring. Tests thankfully revealed no signs of active disease. However, the fear of a flare-up never leaves me. Having Crohn’s has given me so much gratitude for my health.”

How do you balance managing your condition alongside being a parent?
“I became a mum at 40. Oliver is a classic, energetic little boy who currently loves nothing more than to play tag! He keeps me on my toes. Before I had Oliver, I wondered if I could physically cope with having a child. Thankfully, on days when I struggle, I have an amazing support network around me to lend a hand. He knows that sometimes ‘mummy has a poorly tummy and she goes to work to help people with poorly tummies’.”
In our house, we encourage open and honest conversations surrounding poo and our health so that, quite rightly, it’s just seen as an everyday thing. When I’m low, he helps me to see the bright side of life and loves me for who I am, accepting sometimes that mummy doesn’t have the energy to run around!”

What do you wish people understood about digestive conditions, such as Crohn’s disease?
“Having a digestive condition, especially when you’re young, is incredibly tough. However, it’s not the sum of your worth. I wish I hadn’t listened to the negative self-talk. You are not less because of your condition. You are good enough. To live with Crohn’s disease takes a lot of bravery, but it’s not all doom and gloom. It has made me realise my own strength.
My experiences led me to Guts UK, and I’m surrounded by our wonderful community. They give me the courage to be open and honest about my digestive health. We all poo, and it’s so important to do everything we can to reduce the stigma that surrounds our guts.”
Glossary of medical terms:
Adalimumab: A biologic medicine. Biologic medicines target a protein in the body. This protein helps fight off infections but, in some people, it can damage the cells lining the gut. This can cause gut inflammation in people with IBD, so this medicine can help to reduce symptoms.
Colonoscopy: A thin tube with a small camera on the end is inserted via the back passage.
Elemental diet: A liquid diet of prescription supplements, designed to give the bowel a rest, used for some people with Crohn’s disease.
Flare-up: A worsening of symptoms.
Infliximab: A biologic medicine. Biologic medicines target a protein in the body. This protein helps fight off infections but, in some people, it can damage the cells lining the gut. This can cause gut inflammation in people with IBD, so this medicine can help to reduce symptoms.
Iron-deficiency anaemia: A condition where a lack of iron stops the body from producing enough haemoglobin, which is essential for carrying oxygen around the body. More information can be found on the NHS website.
Jejunum: The middle section of the small intestine, primarily responsible for absorbing nutrients and vitamins.
Mercaptopurine: A medicine which reduces the strength of your immune system (immunosuppressant) to reduce inflammation in the gut.
Steroids: Man-made versions of hormones produced naturally by your body, given at a much higher dose. Steroids decrease your immune system activity, which reduces inflammation.
Thalassaemia: A group of inherited conditions that affect a substance in the blood called haemoglobin. Haemoglobin is used by red blood cells to carry oxygen around the body. In people with thalassaemia, some of their haemoglobin does not work properly.
About Guts UK
Guts UK is the national charity for the digestive system and the only UK charity funding research into the whole digestive system.
We provide information and support for people affected by digestive conditions like Crohn’s disease, including a dedicated Helpline.
With your support, we can be there for people like Cherylyn when they need us most.

More support
CCUK is the UK’s leading charity working on Crohn’s disease and other forms of IBD.
Crohn’s In Childhood Research Association (CICRA)
CICRA is the UK’s only children’s IBD charity, providing support and information for young people and their families and funding research to find improved treatments and ultimately a cure.
The IBD Standards say what high-quality care should look like at every point of a patient’s journey – from first symptoms, to diagnosis, treatment, and ongoing care.
IBDesis have created a fantastic video explaining IBD in South Asian languages.



