Helicobacter Pylori (H.pylori)
Download printable versionOverview
H.pylori are a group of bacteria, a type of germ. They live in the sticky mucus that lines the stomach. Up to 2 in 5 people in the UK have H. pylori in their stomach, so it is a fairly common infection of the upper gastrointestinal tract. It also happens more often in people who have learning difficulties, where it can be present in 9 out of 10 people.
H.pylori does not cause any problems for 8 to 9 out of 10 people. One of the main symptoms the infection can cause is indigestion. However, in the majority of patients with indigestion, this is caused by other reasons. Because people can have both it’s easy to assume that one always causes the other. It’s important to check after treatment if the infection has cleared. This helps decide if more tests are needed to rule out other causes. The most common cause of indigestion symptoms is a condition called functional dyspepsia. You can read our information on functional dyspepsia here. However, where H. pylori are found it should always be treated to reduce the risk of complications.
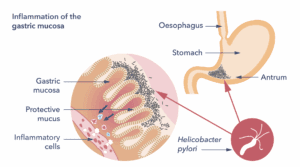
H.pylori infection always causes inflammation of the gastric lining (mucosa). The infection usually starts from the lower part of the stomach (the antrum), but it can then also involve the entire stomach. This generally happens when people take some medications for a long time, for example, proton pump inhibitors (acid blockers). Gastritis is the medical name for inflammation of the lining of the stomach. H. pylori is the commonest cause but there are other causes of gastritis. These include smoking and medicines such as aspirin or certain anti-inflammatory drugs such as ibuprofen or naproxen.
Ulcers: Inflammation due to H. pylori can cause ulcers of the stomach or the first part of the small bowel (duodenum). These are known as peptic ulcers. About 3 in 20 people with H. pylori have ulcers. This is because of the effect it has on stomach acid production and damage of the barrier function of the lining by the chronic inflammation. Although these ulcers tend to cause indigestion and pain, occasionally they become much more serious. They can bleed or even burst (perforate). This happens if the ulcer burrows deep enough into the stomach lining to make a hole. People with ulcers should be tested for H. pylori and treated with the aim of getting rid of the infection if it is present.
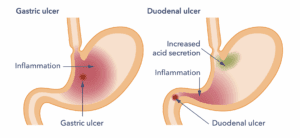
Although H. pylori is a common cause of ulcers, these may also occur because of other reasons. Those reasons are:
- Regular use of certain pain killers such as aspirin, ibuprofen or naproxen. These are also known as non-steroidal anti-inflammatory (NSAIDS).
- Other medicines prescribed for other conditions.
In some people with ulcers, no cause of them can be found. These ulcers are called idiopathic peptic ulcers. Do not stop taking your medicine without speaking to your doctor first. You should always ask your doctor whether any prescribed medicines you are taking may affect your stomach.
Causes
It is not completely clear exactly how H. pylori is passed from one person to another, but a faeco-oral route of transmission is usually proposed. This explains a way infection spreads. H Pylori in poo move from one person to another person’s mouth. It is also unclear why only some people with the infection go on to develop symptoms or further complications such as ulcers.
People who do have H. pylori almost always catch it in childhood when the immune system is not yet mature enough to repel the infection. Transmission occurs usually within families, mostly from parents to children. It stays in their stomach unless it is treated with specific antibiotics.
H. pylori is becoming less common in the UK. Acquiring the infection as an adult is very rare. Once it has been treated and cured, getting infected again is very unusual.
Diagnosis
Breath test
One simple technique to diagnose H. pylori involves a breath test. For this you are given a drink containing a substance called urea. A sample of your breath can be used to check if H. pylori is present in your stomach. The sample is taken before and a short time after drinking the drink. This test is also used to find out whether treatment has been successful, although it needs to be done at least one month after the course of treatment has finished.
Stool test
Stool tests for H. pylori are also now widely used. They are as accurate as breath tests. These involve analysing a small sample of poo for H. pylori proteins. This test can also be used to confirm that infection has been cleared after treatment.
Endoscopy
Doctors can also test for H. pylori during a stomach examination, called an endoscopy. An endoscopy is done using a camera attached to a thin flexible tube. It is passed through the mouth and down into your gullet, stomach and the start of the small bowel. An endoscopy is usually carried out as an outpatient procedure and takes less than 15 minutes. You can choose to have a local anaesthetic throat spray and/or sedative. The endoscopist can guide you in this decision. The procedure is not painful but may be uncomfortable at times. A very small piece of the lining of the stomach (a biopsy) can be taken to test for H. pylori. The biopsy can be used for several different tests to check whether H. pylori is present.
Tests for H. pylori may not be accurate if people are taking certain medicines. Examples are a recent course of antibiotics for any reason within a month of the test. Tests are also not reliable if people have taken proton pump inhibitors (acid blockers). These are medicines which are used to treat ulcers, reflux or indigestion.
Proton pump inhibitors are:
- esomeprazole
- lansoprazole
- omeprazole
- pantoprazole
- rabeprazole
Proton pump inhibitors should not have been taken in the last two weeks before testing. Your doctor will ask that you do not have a test for H. pylori if other medicines you are taking would give a misleading result. If you suspect you take a medicine that might affect the result, please discuss this with your doctor.
If you have indigestion but neither you, nor your doctor know if you have an ulcer:
In the past, most people with severe indigestion often had an endoscopy to look for an ulcer. Now most doctors will check first to see if they have H. pylori. If they do the doctor will treat it with antibiotics.
Generally, if a person has an ulcer and a positive test for H. pylori infection, we know that treating H. pylori is likely to prove successful in healing the ulcer. But it is fair to say that only an endoscopy can confirm whether you have an ulcer or not. Some people without an ulcer may not get full symptom relief by treatment of their H. pylori infection2. People with indigestion who also have other worrying symptoms, will still need to have an endoscopy to rule out other causes of their symptoms, such as:
- Unintentional weight loss.
- Persistently being sick (vomiting).
- Food getting stuck on swallowing or pain on swallowing.
Symptoms
Ulcer complications
The usual symptoms of ulcer complications are severe ongoing indigestion which does not respond to medication and can result in passage of black stools (melaena) or vomiting of blood (haematemesis) or a severe abdominal pain with fever and chills.
H.pylori gastritis symptoms include:
- Belly pain (often a gnawing ache).
- Feeling sick (nausea).
- Belly bloating.
- Burping (belching).
Not all these symptoms might be present. You can read more about indigestion here.
A very small number of people with long standing H. pylori infection may develop stomach cancer. In these people it happens after decades of untreated H. pylori infection. Symptoms that might raise the suspicion of stomach cancer might include:
- Being sick (vomiting).
- Unintentional weight loss.
- Difficulty or pain on swallowing if the cancer sits high in the entry to the stomach.
- A low iron level in the blood (anaemia).
You should contact your doctor urgently for investigation of such symptoms. The risk of stomach cancer increases with age. Please remember that most people will not have stomach cancer. But for those people that do, getting diagnosed sooner is beneficial for treatment.
How might H. pylori affect me over time?
Treatment for the condition is usually very successful. Although sometimes symptoms may take a little time to settle down. Treatment for H. pylori doesn’t always work to get rid of the bacteria. Your doctor should always check to see if H. pylori has gone after treatment. This is done by the testing (see diagnosis section above). If the result is still positive, further treatment is possible.
Before we knew about H. pylori, ulcers could heal up with acid-reducing drugs. But they returned when the treatment was stopped. We now know that treating H. pylori helps ulcers to heal permanently. and therefore greatly reduces the risk of ulcer coming back. All doctors are agreed that people with H. pylori should have treatment.
If the symptoms are due to an ulcer and the H. pylori is treated, most people will recover without further complications. If symptoms are present in people with the infection and no ulcer, some people see a significant reduction in symptoms. Ask your doctor about other possible causes, for example functional dyspepsia, if your symptoms continue.
Treatment
Treatment consists of a combination of 3-4 different tablets. One of these is a tablet to cut down the amount of acid in the stomach, the others are antibiotics. It is the combination that is important in the success of treatment. Traditionally 1-week triple therapy (3 drugs) was used but 2-week triple therapy is now recognised as being more effective. A new medication containing 2 antibiotics and bismuth is now available in the UK. Ten days of treatment with this and a drug to reduce acid is also a useful treatment regimen.
Most people experience no side-effects from treatment but some notice minor problems. Side effects might include:
- A strange taste in the mouth.
- A feeling of sickness.
- A headache.
With one specific antibiotic that is often used called metronidazole, you should avoid alcohol.
Treatment is much more successful if the whole course of tablets is taken exactly as prescribed. Your doctor will encourage you to continue to take the tablets unless the side effects become unpleasant. If you do not complete the course of treatment, the treatment be less successful.
Generally, treatment is always recommended in patients with H. pylori infection, even without an ulcer being present. This reduces symptoms of indigestion in some people. The benefit may not be seen for 12 months but the only way to know if the H. pylori is causing the indigestion is to treat it.
Does H. pylori need to be monitored and, if so, how?
H.pylori should be tested for in first degree relatives of people with stomach cancer. The types of stomach cancer caused by H. pylori include adenocarcinoma and gastric MALT lymphoma. First degree relatives are your parents, brother or sister or children. As the bacteria does cause stomach cancer in a small number of people (between 1 and 3 people out of 100). Discuss this with your GP if this is relevant to you.
Support
Guts UK has further information on indigestion, heartburn, stomach cancer and functional dyspepsia. Contact info@gutscharity.org.uk or call 0207 486 0341 if you would like a copy.
For information, support and guidance, contact our Helpline on 0300 102 4887 or complete our online form here.
What should I ask my doctor?
- Do I need an endoscopy to confirm whether or not I have an ulcer?
- Could my ulcer be caused by something other than pylori?
Discover more:
Copyright © 2026 Guts UK. This leaflet was published by Guts UK charity in November 2025 and will be reviewed in November 2027. The leaflet was written by Guts UK and reviewed by experts in H. pylori and has been subject to both lay and professional review. All content in this leaflet is for information only. The information in this leaflet is not a substitute for professional medical care by a qualified doctor or other healthcare professional. We currently use AI translation tools on our website, which may not always provide perfect translations. Please check for further explanation with your doctor if the information is unclear. ALWAYS check with your doctor if you have any concerns about your health, medical condition or treatment. The publishers are not responsible or liable, directly or indirectly, for any form of damages whatsoever resulting from the use (or misuse) of information contained or implied in this leaflet. Please contact Guts UK if you believe any information in this leaflet is in error.



