Faecal Incontinence
Download printable versionOverview
Faecal or anal incontinence is the involuntary loss of stool, liquid or gas from the bowel. It can often make people feel embarrassed and significantly affect their quality of life. People of any age and any gender may be incontinent, but it becomes more common as we grow older. People with diabetes and neurological conditions are also at risk of faecal incontinence. Faecal incontinence affects up to 1 in 8 people. It is very common but can be under reported as people don’t talk about it. Simple tests can often find the cause and treatment often works to improve incontinence.
Causes
The anal sphincter keeps faeces (poo) inside our bowel until we are ready to pass it. It is formed by a ring of muscles around the last part of the bowel. See the diagram on page 3. The contents of the bowel move along gradually until they reach the rectum. This movement is done by the bowel squeezing and relaxing and is called peristalsis. The rectum acts as a holding reservoir before the faeces or poo exits through the anus. The anal sphincter has two main muscles which keep the anus closed. These are:
- The inner ring, which keeps the anus closed at rest. This is called the internal anal sphincter.
- The outer ring, which is called the external anal sphincter. This provides extra protection when the urge to open the bowel is felt, when we exert ourselves or cough or sneeze.
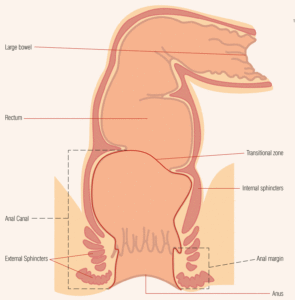
The muscles of the sphincter keep the anus closed until we want to pass faeces (poo). These muscles are controlled by nerves. Some of these nerves detect the sensation of our bowel filling inside. Other nerves are under our conscious control. This balance enables us to stay in control (or ‘continent’). Faecal incontinence happens when this balance is not working correctly.
There are many things that can cause this balance to be upset. Some of them are in the list below:
- People can be born with an abnormal sphincter which is first noticed as a child or teenager.
- Injuries during childbirth such as a tear during labour can damage the sphincter muscles. Symptoms of childbirth injury can sometimes start many years later.
- People of any age who experience an injury or infection of the sphincter can have immediate or long-term effects.
- Problems include Inflammatory Bowel Disease (colitis) and irritable bowel syndrome (IBS). These conditions cause altered bowel function and abdominal pain. They can make the bowel overactive and squeeze at the wrong times.
- Neurological (nerve) illnesses or damage. Neurological issues, such as multiple sclerosis or spinal injuries, can weaken nerve signals to the anal sphincter. This makes it harder to control bowel movements.
- Continence issues can occur following cancer treatment, such as radiotherapy to the pelvic organs.
- Hard poo that is difficult or not fully passed out of the rectum is called constipation. Fluids in the bowel may pass around it. This is called overflow diarrhoea.
- Severe diarrhoea of any cause may cause occasional incontinence.
Symptoms
Faecal incontinence is a bowel symptom. People might not be able to stop the urge to open their bowel. This is called urge incontinence. Some people might not realise they need to open their bowel and are incontinent. This is called passive incontinence.

Diagnosis
You may feel embarrassed about bringing the subject up with your doctor. If you have an in-person appointment, sometimes writing a note and handing it over might help. Your doctor will be comfortable in discussing your problem and will appreciate that it can be difficult for you to talk about. This information lists the types of investigation that might be needed. You may not need all the listed tests immediately, or at all, if symptoms improve. The tests include:
- Physical examination.
- Blood tests and poo tests.
- Tests on how well the anal sphincter is working (anorectal manometry).
- Scans (anal ultrasound).
- A test on how well the muscles and structures of the bowel are working when pooing (defecography).
- Colonoscopy or sigmoidoscopy.
You can request a doctor or healthcare practitioner of the same sex for intimate care treatment or procedures. To help you decide you can also ask about the test and how it will be done.
Diagnosis will depend on how long it has been going on and the pattern of symptoms. At first it will be important for your doctor to take a history. This means going through the story of your symptoms in a structured way.
After this a physical examination is usually carried out. When this is done a doctor or other trained clinician will examine your abdomen (belly). They may also need to examine inside the anal passage. The information the doctor gathers will help plan the next steps.
This might be poo samples to check for blood, infection or other abnormalities. Depending on the results you may then need a colonoscopy or a sigmoidoscopy. This is where the doctor inserts a camera attached to a flexible thin tube through the anus to look inside the bowel. You may need to clear your bowel before the test. Medicine is given before the test to clear the bowel. It is advisable to stay close to a toilet after taking it.
Sphincter function tests may be needed. These tests show how effective the sphincter muscles are at holding in poo. The test checks the strength of the muscles, sensation, and nerve function. Most are simple and quick to perform and are usually pain-free. This testing may use simple pressure measuring devices. These tests are called anorectal manometry.
An anal ultrasound scan can provide a clear picture of both sphincter muscle rings, showing if one or both is damaged. This test may cause a little discomfort, it takes only five minutes and involves no radiation.
Some people will need to have other scans such as an MRI scan.
You may also be asked to open your bowels after some material is inserted into your back passage to assess how you pass stools. This is called deafecography and can be done with x-rays or MRI.
These tests are usually performed in NHS departments with a special interest in continence problems. Your GP can advise on the most appropriate referral for you. Referral can take time – check out the section on support for help with symptoms whilst you are waiting for your appointment. Your GP can also give you information on out how long the wait might be for your appointment and may consider advice or medication if appropriate, while you wait.

How can faecal incontinence affect you?
This condition can often be embarrassing and inconvenient. It can affect all aspects of life, for example work, relationships and social interactions. Simple measures can help make your life a little easier while you are waiting for treatment. These measures could include some of the following things:
- Planning ahead when leaving the house, knowing how long the outing will be and taking a set of spare clothes.
- Finding out where the nearest toilets are. You might find the British Toilet Map useful: https://www.toiletmap.org.uk/.
- Wearing products, such as pads, to help absorb any leakage and protect your clothes.
- It is also important to protect the skin around the back passage by keeping it dry and clean. If you are sore, using a protective cream can help (your pharmacist can advise).
- Guts UK can provide a free Can’t Wait card. This could help you access toilets when out in public. Email us at info@gutscharity.org.uk or call us on 020 7486 0341 if you would like one.
- You could buy a RADAR Key for a small cost, which gives you access to disabled toilets. Several organisations provide them.

Treatment
Any illness that may be causing faecal incontinence should be treated. Medications prescribed for other medical conditions can cause incontinence. It is important to ask a health care professional about this. Other measures improve symptoms for most patients. These may include:
Diet
Changes to diet and bowel habit can be helpful for many people. Some things that we eat and drink can make faecal incontinence worse. These can include:
- A very high fibre diet (too much bran, cereal, fruit etc).
- Too much caffeine. Caffeine is found in coffee. There is a smaller amount in tea. Reduce your intake slowly to decaffeinated options.
- Too much alcohol.
- Large amounts of artificial sweeteners.
Some people find it useful to keep a food diary to help work out which foods trigger their symptoms and may be linked to faecal incontinence.
Medicines
Medicines may be helpful when the bowel is squeezing too strongly when the poo is very loose or when the sphincter muscles are weak.
Loperamide. This works through slowing movement of the intestines when they are pushing the stool around (peristalsis). Loperamide also has the effect of slightly increasing the tone of the anal sphincter, but this is not the main effect. An increased tone may help the muscle to tighten, and this may help improve continence.
Loperamide is not suitable for everyone with faecal incontinence and for a few people, it can be dangerous. It is important to get the advice of a doctor, pharmacist or other qualified prescriber before using it regularly.
If constipation is causing incontinence laxatives or suppositories might be helpful. It may seem counter-intuitive but often harder stool needs loosening with laxatives to then allow overflow to not occur and to achieve a normal consistency bowel motion.
Barrier creams to look after the skin around the back passage can protect from soreness and skin breakdown.

Exercises and biofeedback
Special exercises (pelvic floor exercises) to strengthen the anal sphincter muscles help many people. People can try them whilst waiting for an appointment. Techniques, such as biofeedback, can re-train the bowel. They make it more sensitive to the presence of stool. This teaches you how to contract the sphincter when needed. The service is provided by pelvic floor nurses and some have physiotherapists.
Surgery
Surgical operations can be done to the muscles or the nerves of the anal sphincter. This treatment is not needed for everyone with faecal incontinence. There are many different types of operation, and specialist surgeons can advise about this treatment.
Another therapy called sacral nerve stimulation can be provided in some specialist centres for those where biofeedback did not work or is not possible. This involves stimulating a nerve in lower back to send messages back to nerves in the anal sphincter. This can help some people.
Devices and advice
For a few people, incontinence can be difficult to treat. When this is the case there are things that can help. Some of these allow the bowel to empty at a certain time. There are also anal plugs which can be effective in forming a physical barrier to prevent leakage.
A method called rectal irrigation can help prevent faecal incontinence. This is sometimes called anal or transanal irrigation. Guidelines suggest that if continence cannot be achieved by other treatments, then rectal irrigation should be considered. You would need a referral to a specialist nurse service to receive the correct support. This equipment helps you clear your bowel in the privacy of your own home at a time that is convenient for you. It may take several weeks before a person is comfortable with using the equipment and some people decide to stop using it. This is not the same as colonic irrigation, which is not a recommended treatment.
Your GP can refer you to a continence advisor or other appropriate specialist. Some services may not need a GP referral.
New treatments that are being developed and tested include:
- Treating the muscle fibres of the anal sphincter with radiofrequency so that it works better. This is called SECCA it might not be available everywhere.
- Stem cell injections to improve anal sphincter function.
Support
What to ask your doctor
- What dietary changes would you recommend?
- Do I need medicines?
- Should I be referred for exercise and biofeedback?
- May I be referred to the continence specialist?
If you would like to read some guidelines that healthcare professionals use these are some examples: https://cks.nice.org.uk/topics/faecal-incontinence-in-adults/.
How can faecal incontinence affect me over time?
Long term faecal incontinence can result in feelings of hopelessness. It is important to discuss any low or other feelings with your doctor, so that proper support can be organised. This might involve counselling around specific issues of incontinence for example:
- Anxiety.
- Depression.
- Couples therapy for avoidance of sexual intimacy and relationship problems.
- Maternal childbirth post-traumatic stress disorder (PTSD).
You are also at a higher risk of the skin around the back passage breaking down and developing localised skin infections. This will be noticeable with increased pain when opening your bowels or even just sitting and if left untreated cause you to develop a fever. This can be avoided by keeping the area clean, dry and avoid excessive wiping. Barrier creams such as zinc oxide, incontinence pads and using premoistened tissue and pads for wiping are some ways to help.
If you have had a sphincter injury during childbirth the charity The MASIC Foundation can provide support atmasic.org.uk or by calling 0808 164 0833.
For children with faecal incontinence, further information could be provided by ERIC at https://eric.org.uk/ or by calling 0808 801 0343, Monday to Thursday, 10am to 2pm.
For older adults, Age UK provides various resources and support for individuals dealing with incontinence at https://www.ageuk.org.uk/ or by calling 0800 678 1602 365 days a year, 8am to 7pm.
Bladder and Bowel UK: Visit https://www.bbuk.org.uk/, contact https://www.bbuk.org.uk/enquiries/ or call 0161 214 4591.
According to the Equality Act 2010, incontinence can be classed as a disability. More information can be found here: https://www.gov.uk/society-and-culture/equality. Contact Citizens Advice if you have any questions about work or completing assessment forms https://www.citizensadvice.org.uk/.
If you are experiencing incontinence after childbirth, you might find some useful information from the organisation Pelvic Obstetric and Gynaecological Physiotherapy (POGP).
This leaflet is available in other languages using the accessibility button on our website, by emailing us at info@gutscharity.org.uk or calling us on 0207 486 0341.

Copyright © 2026 Guts UK. This leaflet was published by Guts UK in February 2025 and will be reviewed in February 2028. The leaflet was written by Guts UK and reviewed by experts in faecal incontinence and has been subject to both lay and professional review. All content in this leaflet is for information only. The information in this leaflet is not a substitute for professional medical care by a qualified doctor or other healthcare professional. We currently use AI translation tools on our website, which may not always provide perfect translations. Please check for further explanation with your doctor if the information is unclear. ALWAYS check with your doctor if you have any concerns about your health, medical condition or treatment. The publishers are not responsible or liable, directly or indirectly, for any form of damages whatsoever resulting from the use (or misuse) of information contained or implied in this leaflet. Please contact Guts UK if you believe any information in this leaflet is in error.