Overview
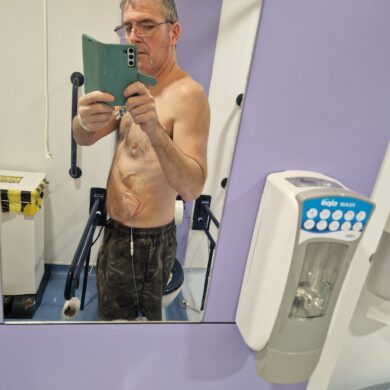
Ascites is the medical term used to describe the build-up of fluid within the belly (abdomen). It is normal to have a small amount of fluid in the abdomen, which is continuously produced and absorbed but when there is an imbalance in this process, fluid can accumulate.
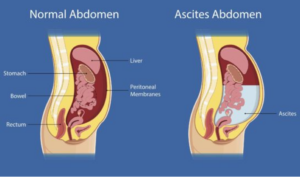
Causes
This is a list of some of the causes of ascites:
- Cirrhosis (severe scarring) of the liver is the most common cause of ascites (up to 8 out of 10 cases).
- Cancers that have spread to the liver or abdomen (about 2 to 3 out of 20 cases). See below for examples.
- Heart conditions (about 3 to 5 out of 100 cases).
- Tuberculosis (about 2 out of 100 cases).
- Kidney dialysis (about 1 out of 100 cases).
- Pancreatic disease (about 1 out of 100 cases).
In the UK, the main causes of cirrhosis are:
- Excessive alcohol intake.
- A build-up of fat in the liver (metabolic dysfunction-associated steatotic liver disease or ‘MASLD’). This was previously called NAFLD by doctors.
- Long-term viral infections of the liver, especially chronic hepatitis B and C
Rarer causes of cirrhosis in the UK include autoimmune liver diseases and inherited diseases. Autoimmune diseases happen when the body’s immune system damages its own liver. An example of an inherited disease is haemochromatosis, which is a build-up of iron in the body.
When cancer is the cause of ascites (including cancers of the stomach, bowel and ovary) it is usually because the cancer has spread to the liver or into the abdomen.
Symptoms
The main symptom of ascites is an increase in the size of the abdomen. Clothes may become tight and belt size may need to increase. If the volume of fluid becomes very large, it can be uncomfortable and make the abdomen feel very heavy or tight. Some people may try to adjust how they stand or walk due to the swelling of the abdomen, which can result in a change of posture. Weight gain caused by the additional fluid may lead to decreased mobility.
The build-up of fluid may put pressure on the bowel. This can cause the person to want to eat less, become constipated or experience a burning pain in the centre of the chest (indigestion). Nausea (feeling sick) and vomiting (being sick) can also occur. There may be an increase in pressure on the lungs or sometimes build-up of fluid in the lungs, causing shortness of breath, especially when lying flat.

Diagnosis
How is ascites diagnosed?
Ascites can be diagnosed by a doctor examining your abdomen, but it is usually confirmed by an ultrasound scan.
An ultrasound scan can help estimate how much fluid there is in the abdomen. It also gives information about the internal organs, especially the liver.
Blood tests will be needed to assess how well the liver is functioning and possibly more detailed imaging tests such as a CT scan or MRI scan.
When ascites is being diagnosed, a sample of fluid will also be taken from the abdomen. This is done by cleaning the skin with antiseptic, injecting a small amount of local anaesthetic (to numb the skin), and then passing a small needle into the side of the abdomen – the procedure is called paracentesis. Sometimes an ultrasound scan is used to decide on the best spot for taking the sample. Paracentesis can cause mild discomfort. If you experience any pain let your doctor know and more pain relief can be given if needed. This fluid sample is analysed to help diagnose the cause of ascites and plan the best treatment.
How can ascites affect you?
Ascites can affect a person in two main ways. The first is its overall impact on your day-to-day life which may include the following symptoms:
- Discomfort and swelling in and around the abdomen.
- Issues with mobility and posture.
- Feeling sick (nausea).
- Being sick (vomiting).
- Shortness of breath.
Feeling embarrassed about how they look might make someone avoid going out in public and stop doing things they enjoy. Fluid build-up should always be reported to your doctor who may recommend a change in treatment or drainage of the fluid.
The other way that ascites can affect you is because of the complications from the actual condition. These include:
- Infection within the fluid. This is called spontaneous bacterial peritonitis (SBP). This can cause abdominal pain, fever, confusion and make people feel very unwell. This is a potentially dangerous complication so if these symptoms occur it is important to get medical attention as an emergency.
- Medicines used to reduce the fluid (‘water tablets’ or diuretics) can cause changes in salt levels in the blood, which may lead to symptoms such as confusion, or problems with kidney function. Therefore, it’s important to have regular blood tests.
- A swelling of the umbilicus (belly button) can occur. This is called an umbilical hernia. Sometimes it may get smaller as the ascites is treated, but occasionally surgery is needed to fix it.
Treatment
Ascites can be treated in various ways, from lifestyle and dietary changes to medicines and medical procedures. The following treatments are for ascites that is not caused by cancer. If you have ascites caused by cancer talk to your cancer team about suitable treatment.

Alcohol reduction and abstinence. You should reduce alcohol drinking to within healthy limits of no more than 14 units per week spread out over 3 or more days. This applies unless your doctor has advised you to stop completely. It is important that reducing or stopping alcohol is done with medical advice and other professional support. People who are dependent on alcohol may have convulsions (fits) if they stop drinking suddenly. Stopping drinking alcohol can be difficult to do, but it can stabilise liver function and help to reduce ascites. People are usually more successful if they have help to stop. Ask your doctor about alcohol support services in your area.
More information on alcohol and the digestive system can be found through this link.
Salt restriction. Salt is found naturally in some foods and is also added to food when eating. Everyone needs some salt but levels in certain foods can be high. Salt contains a chemical called sodium. This is the part of salt that, in large amounts, makes the body hold on to more fluid. Cutting salt to healthy levels can reduce ascites. The best way to do this is to look at the amount of salt on food labels. Most people’s salt intake comes from the salt that is hidden in food. Foods that are high in salt include soups, marinades and sauces, stock, bread, preserved meats and ham, breakfast cereals, some ready meals and snacks.
Reducing the amount of salt in your diet can result in food tasting bland at first. Keep trying and your taste should adjust to a new level. There are some general tips to consider:
- Use a small amount of salt in the cooking water of potatoes and vegetables rather than adding it at the table. Pour away the cooking water.
- Try to avoid adding salt at the table.
- Use herbs, spices and lemon to flavour food instead of salt.
- Compare salt amounts in different foods. There can be a big difference in the amounts. Choose the lower option.
- Avoid using potassium-based salt substitutes or ‘gourmet salts’. These are not better for people with ascites than normal salt. A potassium-based salt substitute could be called potassium chloride, low-sodium salt, low-salt or potassium salt.
- Check tinned food for salt content. Choose lower salt options instead.
- Swap salted nuts for unsalted versions. Choose unsalted crisps and don’t use the salt sachet contained in the packet.
Food labels. Check the ingredients list on food labels. It will help you choose lower salt options. The amount to check per 100g weight of food is:

Sometimes the amount is listed as salt. Salt is also called sodium chloride. Or, it’s just listed as sodium. You should also check how much food you are eating. Some recommended portion sizes are over 100g in weight. In this situation, you could check the front of the label traffic light system. This tells you how much salt is in the recommended portion size. Choose the green options for salt more often and avoid the red options.
The image below shows the nutritional breakdown per portion of the food. If the label is green for salt it is suitable But if you have other restrictions you might have to check if it is suitable for more than one category.
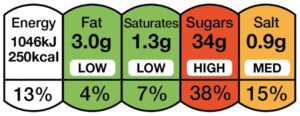
It is not necessary to completely remove salt from the diet. A qualified dietitian will give you advice on how to check this. Ask your doctor for a referral.
Medicine
This will include diuretics (water tablets) that stimulate the kidneys to remove more of the fluid in our bodies by making more urine. These will usually need to be taken one or more times daily.
Beta blockers are medicines that may be used for some people where the pressure is raised in the blood vessels around the liver.
Antibiotics will be used to treat infection in the fluid. (see above). Some people may need to take antibiotics all the time to prevent infections. These are called prophylactic antibiotics. The use of regular antibiotics to prevent infection are only considered in specific situations when the risk of serious infection is high. The benefit of this treatment generally outweighs any risks of regular use, but if you have concerns talk to your doctor about your treatment.
Other medicines may be needed for individual people with ascites.
Treatments in hospital
Some people with severe ascites will need fluid drained from the abdomen to reduce the amount. Doctors call this large volume paracentesis (LVP) or an ‘ascitic drain’. The drain usually stays in for about 6 hours to allow the fluid to drain out of the abdomen, then it is removed. For some people, this may need to be done regularly if the ascites keeps on re-accumulating.
To help correct the mineral and protein balance of the body, intravenous fluids containing proteins such as albumin may need to be given into a vein by a drip.
A specialised procedure where a tube (stent) is inserted between two of the large veins of the liver may be used to improve the flow of blood back to the heart. This reduces the blood pressure in the veins and helps to prevent fluid build-up. This is called a transjugular intrahepatic portosystemic shunt (TIPSS).
A small, battery-operated pump can be placed under the skin to automatically and continually move ascites fluid from the abdomen into the bladder. This is known as an automated low-flow ascites pump (ALFAPUMP).
Liver transplant. If the ascites is caused by liver problems then a liver transplant may be needed. This may not be a suitable treatment for all people with ascites. Your doctor can discuss the options with you at the time if it becomes an option. It is usually considered when other treatments for ascites have stopped working and the liver damage is severe. If you have a dependency on alcohol or drugs you will have to address this to be considered to go on the transplant list. There is help available for you to stop any dependency. Ask your doctor to be referred to substance use disorder services in your area.
Does ascites need to be monitored and, if so, how?

Yes, it does need to be monitored so that you receive the right treatment.
Regular measurements of weight and abdominal size are useful ways to monitor the volume of fluid as rapid weight changes can indicate fluid loss or gain. If you feel your weight is changing very quickly you may need to see a doctor for a check-up.
Whilst taking diuretic medicine, it is important to have regular blood tests to monitor salt levels and kidney function. If diuretics have only just been started, these blood tests will occur more frequently until the body is used to the medicine.
How can ascites affect you over time?
This largely depends on the underlying cause. The majority of people with ascites caused by cirrhosis will respond to treatment. However, some people will not respond to medicine or dietary changes and may continually re-accumulate fluid in their abdomen. In this case, repeated drainage of the fluid may become necessary.
Knowing you have ascites can be a worrying time. Being well informed and following the advice from your healthcare professional can help you to understand what is happening and have the knowledge you are doing all that you can to support your health. If you have any questions about what to expect in the future your doctor is the best person to advise you.
Support
What to ask your doctor?
- Do I need to avoid any foods? Do I see a dietitian or is there a diet sheet?
- Does developing ascites mean my condition is worsening?
- Does the fluid need to be drained? What specific symptoms should I look for to know if drainage is needed – is measuring my weight helpful?
- Are there any medicines I can take? Do the medicines have any side effects?
- What support should I need at home? Can you help to provide this?
Other organisations that can help. The British Liver Trust at British Liver Trust – Pioneering Liver Health provides information and support to people with Liver disease.
If you have cancer as a cause of your ascites then you can find support from MacMillan or call 0808 808 0000 8am to 8pm.
Other information which is not gut related is available from the condition pages on the NHS website. These pages do have links to the relevant support organisations.
Current medical guidelines
The current guidelines from the British Society of Gastroenterology on the diagnosis and treatment of ascites can be viewed by this link.
Research
What more research needs to be done on ascites?
Further research is necessary to find new medications that are more effective at reducing ascites and have fewer side effects – clinical trials of potential medicines are ongoing. In addition, research into cirrhosis and the spread of cancers could help to find new ways to prevent or control ascites.
Discover more
Copyright © 2026 Guts UK. This leaflet was published by Guts UK in February 2025 and will be reviewed in February 2028. The leaflet was written by Guts UK and reviewed by experts in ascites and has been subject to both lay and professional review. All content in this leaflet is for information only. The information in this leaflet is not a substitute for professional medical care by a qualified doctor or other healthcare professional. We currently use AI translation tools on our website, which may not always provide perfect translations. Please check for further explanation with your doctor if the information is unclear. ALWAYS check with your doctor if you have any concerns about your health, medical condition or treatment. The publishers are not responsible or liable, directly or indirectly, for any form of damages whatsoever resulting from the use (or misuse) of information contained or implied in this leaflet. Please contact Guts UK if you believe any information in this leaflet is in error.