Overview
Achalasia means a lack of relaxation from the Greek word ‘chelasis’. It is a progressive condition that affects the nerves and muscles of the oesophagus (gullet or food pipe). It mainly affects the lower end where it meets the stomach. Achalasia holds up the passage of food and fluid down the oesophagus and prevents it entering the stomach. It is very rare with approximately 2 to 3 in 200,000 people diagnosed each year. This is the same as 2 to 3 people being diagnosed in a large town. It is a condition specific to the oesophagus and doesn’t affect any other sites in the gut. It can affect all ages. In children, 1 in 263,200 are diagnosed. This is the same as one child being diagnosed in a large town. The average time for an adult to be diagnosed is 15 years.
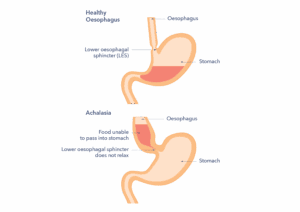
Causes
Achalasia is both a problem with the movement of the muscles in the oesophagus and the function of the lower oesophageal sphincter. The lower oesophageal sphincter is a band of muscle. It is found between the bottom of the oesophagus and the stomach. It acts like a valve, preventing food and fluid from going back up the oesophagus. Achalasia occurs when the nerves and muscles of the lower part of the oesophagus waste away. This causes an inability of the lower oesophageal sphincter to relax. This prevents food and fluids from entering the stomach. Also, the muscles of the oesophagus lose their ability to squeeze in a coordinated way. This further impairs the passage of food down the oesophagus. Over time, the oesophagus can become enlarged (dilated). In most cases, the cause of achalasia is unknown. It might be caused by an infection or an autoimmune condition, but more research is needed to know for sure.
There are three types of achalasia:
- Type 1: The muscle squeezing that normally happens to move contents through doesn’t and the sphincter doesn’t relax as it should.
- Type 2: Pressure builds up in the oesophagus when people swallow.
- Type 3: The muscles sometimes go into spasm when people swallow.
Some people can have more than one type of achalasia.
Symptoms
The most common symptom of achalasia is difficulty swallowing (dysphagia) that occurs with both food and liquids. Food may feel as if it is stuck in the oesophagus after eating, causing chest discomfort or pain. The symptoms may be present for months or even years before the patient seeks help. Regurgitation of food (bringing food back up) may occur as food is retained in the oesophagus and has nowhere to go except upwards. This can cause choking or coughing and may lead to chest infections if the food goes back down the wrong way and into the lungs. As a result of food not passing into the stomach and difficulty swallowing, less food is ingested and it is common to lose weight. Sometimes, no symptoms are experienced and the condition is diagnosed incidentally during tests for a different condition.
Diagnosis
How is achalasia diagnosed?
Achalasia is a rare condition with non-specific symptoms that can be challenging to diagnose. If your doctor suspects you might have achalasia, they will recommend several tests to confirm the diagnosis. Each test is straightforward and typically performed in a clinical setting. Your healthcare team will guide you through the process and provide any necessary support to ensure your comfort. Understanding these tests can help you feel more prepared for your journey to diagnosis. If you have any questions or concerns, don’t hesitate to talk to your doctor.
Endoscopy
This is where a small tube with a camera on the end is inserted into the oesophagus and stomach via the mouth. The tube is as wide as a small finger. Some clinics are using a camera that is inserted through the nose instead. The test is useful if the doctor suspects a different cause of symptoms.
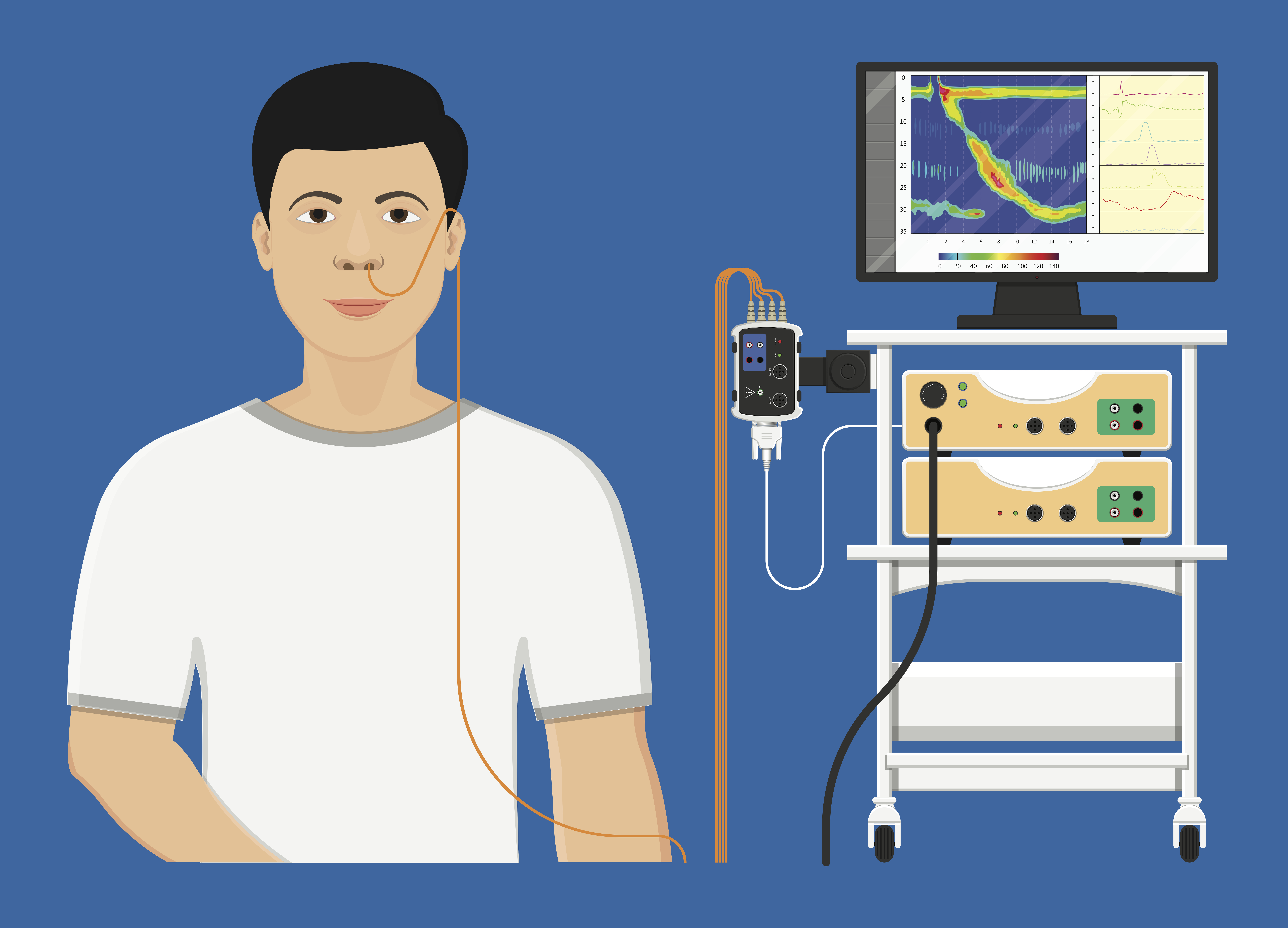
Oesophageal manometry
The muscles in the oesophagus create pressure to push food down. Oesophageal manometry measures the pressure waves. It is the main investigation for the diagnosis of achalasia. A small plastic tube holds pressure sensors. It is placed into the oesophagus via the nose. Over thirty minutes, the sensors read the function of the oesophagus. This detects any abnormalities.
Barium swallow
This test involves drinking a white liquid. This is called barium. Barium coats the oesophagus. It shows the shape/outline of the under X-ray or other examination. This test can be helpful alongside manometry. This can show whether there is a widening of the oesophagus. This is called mega-oesophagus (see below).
How can achalasia affect you?
Achalasia can affect you in two main ways. The first and most common is the effect on the quality of a person’s life due to difficulty swallowing, which can affect a person’s ability to go out for meals or eat the same things they are used to. Achalasia can also affect a person’s weight and nutrition. If you are unable to maintain a healthy weight and become malnourished, other feeding methods may be needed. For example, nasogastric feeding. This is where feed is pumped through a tube which is placed into the stomach via the nose. Chest infections that occur from regurgitation of food can be a problem.
The other way that achalasia can affect you is because of the complications from the actual condition. These are both very rare and include:
End stage achalasia
Doctors would call achalasia ‘end stage’ when the more common treatments have not been effective. The oesophagus can also stretch – see below. If the person would benefit, surgery to remove the oesophagus might still be offered. This is called an oesophagectomy (see treatment section).
Mega-oesophagus
Over a long period of time the oesophagus can stretch until it becomes very wide. When the muscles cannot stretch anymore the oesophagus can tear or burst. Symptoms can include:
- Sudden onset abdominal/chest pain that can be felt as a tearing pain.
- Bringing up blood
- Becoming very unwell very quickly.
This is a medical emergency.
Cancer of the oesophagus
Achalasia can rarely be associated with developing this cancer. This risk is one of the reasons you should remain under follow-up with a specialist. 13 out of 1000 people with achalasia in the UK may go on to develop oesophageal cancer in the future. Figures are similar to one person in a small town being diagnosed.
Treatment
There are several treatment options. These include medicines, endoscopy procedures or surgery. Unfortunately, treatments can’t cure achalasia. They can however significantly help with symptoms. The aim is to relax the sphincter so that food can pass into the stomach. The outcome of different treatments can vary. Likely benefits and risks can also differ. This depends on some factors.
The best option is to discuss the best management of your individual condition and personal circumstances with your specialist. This takes into account the following factors:
- Whether you are fit enough to undergo the treatment, for example surgery. Other options are available if you are unable to have surgery. Previous medical history which includes any other health conditions might impact choice and treatment risk.
- Time to diagnosis. The duration of symptoms before receiving a diagnosis may affect the disease’s progression and treatment efficacy.
- Personal choices around treatment and lifestyle considerations play a role in deciding the most suitable treatment plan.
Choice of treatment depends on if the person chooses that option and if they are fit to undergo the treatment. The first three treatments have similar benefit and are recommended:
Dilatation
This is where the sphincter is stretched open using a small balloon. The balloon is passed via an endoscope, a thin tube with a camera at one end. This is done using sedation or general anaesthetic. Once in position, the balloon is inflated. The inflation stretches and breaks the fibres in the sphincter. It relieves symptoms in about 9 out of 10 people with achalasia in the first year. 1 in 3 people might have a recurrence in 4 to 6 years of treatment. Sometimes more than one procedure may be needed. There are some risks, particularly of perforation, or a hole in the gullet. Perforation may happen in 2 to 4 people in 100 people who have the procedure. Your doctor will explain the risks to you before the procedure.
POEM (Per-Oral Endoscopic Myotomy)
This is an endoscopic treatment. It is performed under general anaesthesia. It involves making cuts to the lower oesophageal sphincter muscles. This makes them looser and improves swallowing. Because it uses an endoscopy, it is less invasive than Hellers Myotomy (see below). Complications of the POEM procedure include perforation. 3 out of 10 people might also develop acid reflux. Both of these will need further treatment.
Surgery
A procedure called a Heller’s Myotomy is used. This cuts the muscle fibres of the sphincter. The aim is to permanently improve swallowing. This procedure is performed using keyhole surgery (laparoscopy). A Heller’s Myotomy is likely to cause GORD (chronic acid reflux). Because of side effects of GORD, it is often combined with another surgery. This is called a partial fundoplication, which reduces acid reflux symptoms. Complications of this can include perforation and bleeding.
Botox
This is a substance called Botulinum toxin. It is injected into the sphincter, at the time of the endoscopy. This relaxes the muscle fibres in the sphincter. It does this by temporarily paralysing nerves that signal the sphincter to contract. It can help with symptoms for anywhere between a few months to one year. It is not a permanent treatment and usually has to be repeated. However, if the person is unfit for other treatments or chooses this procedure, it is a useful and relatively safe approach.
Medications
Some medications may be used but they are not as effective as the other treatments. Medications are not recommended by recent guidelines.
Oesophagectomy
This is surgery to remove the gullet. This surgery should only be considered as a last resort when other treatments are of no benefit. There are common longer term side effects with this kind of surgery, and this includes:
- Dumping syndrome: Please see Guts UK’s information on dumping syndrome, available to download here.
- Having to eat smaller meals more frequently: This is because oesophagectomy surgery affects the capacity of the stomach. After surgery, there will be immediate changes to the texture of foods that you can eat and there are also some foods that some people struggle to eat. A dietitian should be involved in helping you eat after the surgery.
Your surgeon can discuss the risks and benefits of this kind of surgery with you, including more immediate surgical risks.
Other treatment side effects
A common complication of achalasia treatments is acid reflux (GORD). This can in most instances be managed easily with acid-reducing medication.
- Ensure that food is chewed well.
- Eat sitting upright.
- Sleep with a few pillows so you are not completely flat or use a wedge pillow.
- Avoid eating within three hours of bedtime.
If you experience heartburn or pain, your doctor can prescribe medicines to help.
Does achalasia need to be monitored and if so, how?
As mentioned above, it is important to monitor symptoms and have regular follow-up visits. It is essential to attend appointments to ensure treatment is commenced when required to prevent symptoms becoming worse. If you are struggling with your food or fluid intake, ask your doctor for a referral to a dietitian.
No specific monitoring is needed for the low risk of associated cancer. However, let your doctor know as soon as you can about any changes in symptoms and they can refer you for investigation.
Support
Unfortunately, there is no cure for achalasia. Some people will achieve reasonable symptom control with treatment. But others might have ongoing symptoms despite treatment.
What to ask your doctor?
- What lifestyle changes can I make to support my treatment and improve my symptoms?
- Can you explain the potential risks and benefits associated with the recommended treatments?
- May I be referred to a dietician to see if there are any changes I can make to my diet that may help with my symptoms?
- Should I keep a food or symptom diary to help track changes and see what might be triggering my symptoms?
- How often do I need follow-up?
- Which is the best treatment for me in the long term?
Other support
To connect with others and for further support, visit the website for the charity Achalasia Action.
Learn more about achalasia
Copyright © 2026 Guts UK. This leaflet was published by Guts UK in August 2025 and will be reviewed in August 2028. The leaflet was written by Guts UK and reviewed by experts in achalasia and has been subject to both lay and professional review. All content in this leaflet is for information only. The information in this leaflet is not a substitute for professional medical care by a qualified doctor or other healthcare professional. We currently use AI translation tools on our website, which may not always provide perfect translations. Please check for further explanation with your doctor if the information is unclear. ALWAYS check with your doctor if you have any concerns about your health, medical condition or treatment. The publishers are not responsible or liable, directly or indirectly, for any form of damages whatsoever resulting from the use (or misuse) of information contained or implied in this leaflet. Please contact Guts UK if you believe any information in this leaflet is in error.




