Biliary Sphincter Disorders
Download printable versionOverview
This information is about Biliary Sphincter Disorders, formerly known as Sphincter of Oddi Dysfunction.
When we eat, our bodies carry out many different processes which help us digest and absorb all the nutrients we need. One stage of the digestion process is the production of bile, a substance produced by the liver, which plays a large role in the digestion of fats. It is transported from the liver to the gallbladder, where it’s stored, ready for when we next eat.
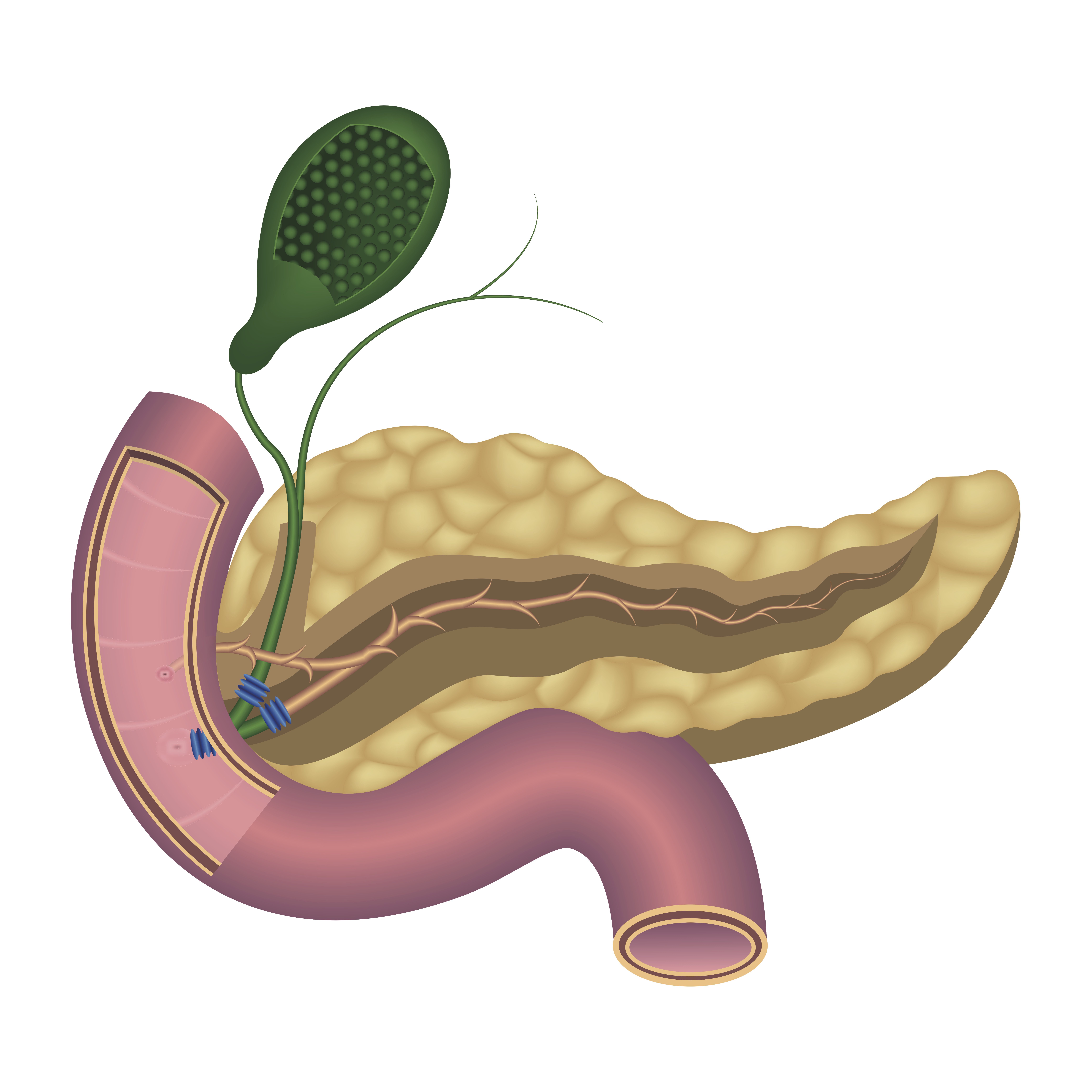
Chemical signals called hormones tell the gallbladder when to work, it then starts to contract and squeeze the stored bile into the common bile duct. The common bile duct is around 7cm long and at its distal end (the bottom) it meets with the main pancreatic duct – which transports the vital digestive enzymes lipase, amylase and protease, produced by the pancreas. When these two main ducts join, a tiny duct forms called the Ampulla of Vater.
The juice made up of the bile and pancreatic enzymes continue through the Ampulla of Vater and out into the first section of the small intestine called the duodenum. Here it begins mixing with the partially digested food from the stomach, and digestion continues. This process relies on a small ring of muscle wrapped around the end of the ampulla of Vater duct to work efficiently, controlling the flow of juices into the duodenum by relaxing and contracting at the right time. This small muscular valve is commonly known as the Sphincter of Oddi.
If the Sphincter of Oddi doesn’t relax appropriately, the duct can stay tightly closed or spasm, which stops the flow of the juices into the duodenum. These juices can then back-up, causing the pressure inside the ducts to increase. When this happens, symptoms can develop, including severe attacks of abdominal pain and nausea.
Biliary Sphincter Disorders occur almost exclusively in people who have had their gallbladders removed (an operation called a cholecystectomy). Around 70,000 people undergo this operation every year in the UK and it is estimated that up to 5-10% will suffer long-term symptoms. Although considerably less common, people who still have their gallbladders can also suffer from Biliary Sphincter Disorders.
There have been many terms used to describe problems – or suspected problems – of the sphincter of Oddi, including post-cholecystectomy syndrome and more recently Sphincter of Oddi Dysfunction (SOD). Depending on the symptoms and various test results, SOD consisted of three sub-groups, Types I, II, and III.
After many years of studies, including trialling different treatment options for all types of SOD, it has become apparent that the management and treatments used is not a ‘one size fits all’, despite people suffering from the same, sometimes extremely debilitating, symptoms.
Therefore, a new classification system for Biliary Sphincter Disorders has been developed. It’s hoped that the new system will help reduce any confusion and frustration, and most importantly, make sure people are getting the appropriate medical care and support they need.
The new classifications are as follows:
- Biliary Sphincter Stenosis/Obstruction: Certain abnormalities are detected when the sphincter doesn’t function correctly due to stenosis (narrowing) or obstruction. These include blood test results showing raised liver or pancreatic enzymes and scan images showing dilation (widening) of the common bile duct or main pancreatic duct. It can lead to attacks of pain or recurrent acute pancreatitis.
- Functional Biliary Sphincter Disorder: Although some abnormalities are evident – either dilation of a duct or raised liver or pancreatic enzymes – they may not necessarily warrant invasive intervention. Studies have repeatedly shown that the risks of invasive procedures for some people with Functional Biliary Sphincter Disorder outweigh the benefits, and can result in long-term problems.
- Functional Biliary Sphincter Pain: Where the liver enzyme tests are normal, and tests do not show any bile duct abnormality to explain the symptoms of biliary pain.
Causes
Biliary Sphincter Stenosis/Obstruction (formerly known as SOD Type I) occurs when the sphincter loses the ability to relax and open the duct properly. One of the most common causes is when a gallstone(s) becomes trapped in the common bile duct after being ejected from the gallbladder, which can lead to permanent scarring (fibrosis) and damage to the sphincter and duct. Other causes of biliary sphincter stenosis include gallbladder disease, gallbladder surgery and procedures such as cholecystectomy and ERCP, pancreatitis, and cholangitis (inflammation of the bile duct).
The causes of Functional Biliary Sphincter Disorder & Functional Biliary Sphincter Pain (previously SOD Type II and Type III, respectively) are not always clear, even when an abnormality is evident in functional biliary disorder. One theory as to why post-cholecystectomy patients are more commonly affected, is that nerves are damaged during the surgery, and this damage affects how the sphincter functions. When no mechanical abnormalities are apparent as to why the sphincter doesn’t work correctly, it’s known a functional disorder.
Functional Biliary Sphincter Pain and the Central Nervous System (CNS)
There are many unknowns when it comes to the science of pain, however, we know that just a very slight flaw in the complex communication system between the brain and the gut, including the sphincter of Oddi, can affect how we perceive pain. An example of this is central sensitisation. This is a condition where there is an increased responsiveness in the brain to normal or near normal inputs from the peripheral nervous system. Pain receptors (nociceptors) detect when something is happening to the body that needs our attention, for example, an inflamed internal organ or a broken leg, then sends signals to the brain to warn us. The pain receptors and signals correspond to the type and severity of the damaged tissue. Sometimes these receptors become hypersensitive and more reactive, and the pain we experience is amplified and more severe (known as hyperalgesia).
We often hear how demoralising and frustrating it can feel when there are no obvious causes as to why someone is experiencing such pain, and start thinking that it must be ‘All in their head’! The human body is a very complex machine, and even with the absence of abnormal scans and blood test results, it doesn’t mean the pain is any less real for the sufferer.
Once again, this is why it’s imperative that people receive the correct care and support for their individual needs.
Medications
Certain medicines can exacerbate sphincter pain in some people, and common drugs known to cause the sphincter to spasm – and consequently cause pain – are morphine-based opioid drugs. If you’re prescribed any medication which you believe may be causing more pain and symptoms, you must seek medical advice. Speak with your GP or specialist consultant before stopping any medication, as this can cause unwanted side effects.
Symptoms
The most common symptom (for all 3 types of SOD) is abdominal pain in the upper right section of the abdomen, after eating – with particular link to fatty foods. The pain occurs just underneath the right side of the rib cage, lasts at least 30 minutes, is not improved by bowel movements or changes in posture and can be severe enough to affect daily activities.
Occasionally, the pain may radiate around to the back and be severe enough to wake people with biliary sphincter disorder up at night. It is rarely a daily or constant pain. The symptoms may come and go and vary in severity.
Symptoms can also mimic other, more serious, conditions, such as pancreatitis (inflammation of the pancreas), cholecystitis (inflammation of the gallbladder), cholangitis (inflammation of the bile duct), plus other functional gastrointestinal conditions like irritable bowel syndrome (IBS), and centrally mediated abdominal pain syndrome (CAPS).
The pain lasts anywhere between 30 minutes to several hours and can be so severe that it wakes people from their sleep during the night. Consequently, this can have a massive impact on a person’s everyday activities, and life in general. Although the attacks can be painful and can last some time, it is rarely a constant, chronic pain. Unlike some other gastrointestinal conditions, the pain and symptoms aren’t relieved by having a bowel movement.
Other symptoms include nausea, vomiting, weight loss, and diarrhoea. Diarrhoea could also be due to a condition called bile acid malabsorption (BAM) and is seen in some people who have had their gallbladder removed. Read our information on BAM and ask your doctor if you feel this is the case.
Diagnosis
Diagnosis of Biliary Sphincter Stenosis/Obstruction
There are various diagnostic tests used to determine if a person’s symptoms are due to a Biliary Sphincter Disorder. These tests include:
- Blood tests: to measure the levels of liver and pancreatic enzymes in the blood. The liver enzymes include aspartate aminotransferase (AST), alanine aminotransferase (ALT), and alkaline phosphatase (ALP). The pancreatic enzymes are lipase and amylase (you may see these written as ‘serum amylase’ and ‘serum lipase’ which means the levels detected in the blood: serum means blood fluid).
- Imaging techniques: Together with the blood tests, scans are used to detect any abnormalities of the bile duct, sphincter of Oddi, liver, pancreas, and gallbladder (if still present). The scans commonly used include abdominal ultrasound, CT scan, EUS (endoscopic ultrasound), and MRI. You may also come across the term MRCP (magnetic resonance cholangiopancreatography) which is a specialist name for an MRI scan that takes images specifically of the gallbladder, bile ducts, liver, pancreas and pancreatic ducts.
- Hepatobiliary iminodiacetic acid scan (HIDA): also known as cholescintigraphy or hepatobiliary scintigraphy, is a nuclear medicine scan used to follow the flow of bile from the liver – where it’s produced – to the small intestine. A radioactive tracer is administered into a vein, then taken up by the liver, and secreted with bile. The bile is then clearly seen on the scan, and any constrictions or blockages of the liver, gallbladder, or biliary tract are detected. HIDA scans are generally used in diagnosing gallbladder disease but are sometimes used to detect biliary abnormalities, despite some limitations.
To diagnose Biliary Sphincter Stenosis/Obstruction, blood test results will show raised levels of liver and/or pancreatic enzymes during or soon after a painful attack. There will also be evidence of a ductal abnormality on scan images, showing dilation of the common bile duct and/or main pancreatic duct. When the Sphincter of Oddi is obstructed due to fibrosis, the build-up of pressure and digestive juices in the ducts increase, causing the ducts to widen (dilate). Apart from the ductal dilation and thickening of the Sphincter of Oddi, no other biliary or pancreatic abnormalities will normally be present.
Diagnosis of Functional Biliary Sphincter Disorder
The tests used to diagnose Functional Biliary Sphincter Disorder are the same as the ones used in diagnosing Biliary Sphincter Stenosis/Obstruction (see above). However, a diagnosis may be made if there’s evidence of either raised liver and/or pancreatic enzymes or abnormal scan results (showing a dilated duct).
Diagnosis of Functional Sphincter Pain
We know that Biliary Sphincter Disorders are most prevalent in people – predominantly females – who have had their gallbladders removed (cholecystectomy). If pain and symptoms continue after surgery the possibility of a Biliary Sphincter Disorder should be investigated. Tests will also be used to rule out more serious conditions.
If blood tests, including checking for raised liver and/or pancreatic enzymes are normal, and scan results show no abnormalities of the common bile duct and/or main pancreatic duct, a diagnosis of Functional Biliary Sphincter Pain may be made.
Treatment
Treatment of Biliary Sphincter Stenosis/Obstruction
Medications
Although medication treatments are still quite limited, there are various types that can help with the pain, the motility of the sphincter (how the muscle works), and other symptoms such as nausea and vomiting (see below).
These medicines include: various types of anti-depressants that are well known to modulate pain perception (inhibit and reduce pain signals) including tricyclic antidepressants e.g. amitriptyline, and serotonin-norepinephrine reuptake inhibitors (SNRIs) e.g. duloxetine; calcium channel blockers such as Nifedipine which have a relaxing effect on the sphincter and helps prevent the spasms; and antispasmodics/anticholinergics such as Buscopan (hyoscine butylbromide) which can also help in relaxing the sphincter.
Important note: If you’re prescribed any medication which you believe may be causing more pain and symptoms, you must seek medical advice. Speak with your GP or specialist consultant before stopping any medication, as this can cause nasty unwanted side effects.
Endoscopic retrograde cholangiopancreatography (ERCP)
One of the of the main procedures used to treat Biliary Sphincter Stenosis/Obstruction is called an endoscopic retrograde cholangiopancreatography (ERCP). An ERCP involves using a long flexible tube, around the width of your little finger, called an endoscope. This is fitted with a small camera and light which assists the doctor as it’s inserted through the mouth, and carefully guided down the oesophagus and through the stomach until it reaches the duodenum – the first section of the small intestine. There is a small opening on the side of the duodenum called the major duodenal papilla, and it’s through this opening where the digestive juices enter the duodenum. Once the endoscope is in position, the doctor passes extremely small instruments down the scope and through the major duodenal papilla, where they reach the Sphincter of Oddi, Ampulla of Vater, and both the common bile duct and the main pancreatic duct.
Enabling the sphincter to relax, and the duct to open better, can be achieved by cutting the muscle fibres of the sphincter – a procedure called an endoscopic sphincterotomy. Other procedures can be performed via ERCP including endoscopic balloon sphincteroplasty (also known as balloon dilation) – when a tiny un-inflated balloon is inserted into the duct where the obstruction is, and then slowly inflated causing the sphincter and duct to open, and allowing the juices to flow more easily. Endoscopic balloon sphincteroplasty can also be used to remove stones from the common bile duct.
Bile duct stents (biliary stents): thin hollow plastic or metal tubes can be inserted via ERCP, and are also used to keep an obstructed duct open. Whilst in the duct, the digestive juices can continue to flow through the middle of the stent freely. Stents are also used as a preventative treatment after endoscopic sphincterotomies. Accessing the ampulla of Vater through the major duodenal papilla, and cutting the sphincter, can result in inflammation which subsequently blocks the pancreatic duct and can lead to post-ERCP acute pancreatitis. By inserting the stent after the cut, it keeps the duct open until the inflammation is resolved. In most cases, the stent will eventually fall out of the duct and is excreted from the body during a bowel movement – without even knowing!
Treatment of Functional Biliary Sphincter Disorder
The main treatment of Functional Biliary Sphincter Disorder can include:
Dietary Changes
Although dietary triggers can vary greatly from person to person, some dietary changes may be very beneficial. Keeping a food diary can also be very helpful. Of course, maintaining a healthy balanced diet is paramount, so a referral to a specialist dietician is often advised.
Pain Relief
Pain is the most common symptom of all Biliary Sphincter Disorders, and in many cases the hardest symptom to manage. Traditional drugs used to treat pain – ranging from over-the-counter pain relief to much stronger prescription drugs – aren’t always effective and in some cases can make the sphincter pain worse, for example, morphine-based opioids. Although there may be times when these strong drugs may be needed, they also come with their own adverse side effects, including nausea, constipation, increased pain, and long-term dependency. As mentioned above, other drugs are successfully used in helping manage the pain, including various types of anti-depressants, calcium channel blockers, and antispasmodics/anticholinergics.
Cognitive behavioural therapy (CBT)
Activities to improve cognitive function may also be beneficial in helping to manage – and learn to live with – pain, such as cognitive behavioural therapy (CBT) and meditation techniques including mindfulness. A lot of people won’t see how these could help with their debilitating pain, and consequently think that they’re not being listened to. That is not the case. This therapy can be extremely beneficial, especially when used together with the other treatments.
Pain clinic
Your GP or hospital consultant may refer you to a pain clinic. These clinics are made up of teams who are experts in the field of pain, and include specialist doctors (often anaesthetists), clinical nurse practitioners, psychologists, occupational therapists and physiotherapists.
Anti-sickness medication
Nausea and/or vomiting can also have an impact on a person’s day-to-day general activities, and to help with this there are various anti-sickness drugs (antiemetics).
Watch and wait
Regular monitoring of the symptoms along with imaging of the bile duct to see if there are any changes. If the symptoms persist then the people with biliary sphincter disorder may be referred to a specialist clinic for further investigation.
ERCP Procedures
As already discussed, procedures carried out via ERCP aren’t always performed for patients with Functional Biliary Sphincter Disorder due to the results of studies and the benefits versus the risks. Each patient is assessed individually and a decision will be made on their own clinical presentation.
Botox
If an ERCP is advised, Botox could be the first treatment option. This involves injecting the sphincter with the neurotoxin Botulinum toxin (Botox) – the same toxin used in cosmetic and other medical treatments – which inhibits the sphincter from contracting and closing the duct tightly.
Treatment of Functional Sphincter Pain
As with functional biliary sphincter disorder, functional biliary sphincter pain is treated on a symptom-by-symptom basis. However, unlike functional biliary sphincter disorder, ERCP is not considered for diagnosis or treatment, as it does not help improve the symptoms. In this situation medications such as neuromodulators may be considered, Amitriptyline, and serotonin- norepinephrine reuptake inhibitors (SNRIs) e.g. Duloxetine may be triedor you may be referred to specialist pain or psychotherapy services.
Support
Functional Biliary Disorder can impact a person in many ways including its overall impact on general wellbeing due to the symptoms, which can be long term and frequent. It is recognised that ongoing symptoms with no clear cause can cause major upset, and feelings of hopelessness amongst many people with biliary sphincter disorders. If any of these feelings are experienced, it is important to let the doctor know so that appropriate support can be organised.
Do Biliary Sphincter Disorders need to be monitored?
- Biliary Sphincter Stenosis/Obstruction: If dilation or sphincterotomy have been carried out, then usually one follow up appointment with the specialist who carried out the procedure should be sufficient to establish whether it has been a success. Recurrent symptoms can occur if there is scarring of the incision made during endoscopic sphincterotomy or surgical sphincteroplasty. If pain is still present, then another diagnosis should be considered.
- Functional Biliary Sphincter Disorder and Functional Biliary Sphincter Pain: If the symptoms of Functional Biliary Disorder are well controlled, then regular follow-up with a doctor is not necessarily required. However, in many cases the symptoms can come and go, in which case regular follow-up would be useful to ensure that new treatments for symptom control can be considered.
What to ask your doctor when you see them?
Functional Biliary Sphincter Disorder:
- If I need an ERCP can I be referred to a specialist unit?
Functional Biliary Sphincter Pain:
- May I be referred to a dietitian to see if there are any changes to my diet that may help with my symptoms?
- Which treatment option is best for me?
- May I be referred for specialist pain or psychotherapy services?
Research
Further research into the underlying causes of Biliary Sphincter Disorders may help the development of more targeted treatments. This includes exploring better medical therapies for people with biliary sphincter disorders and more targeted psychological support. There also needs to be a better understanding about the long-term outcomes with these disorders.
DISCOVER MORE:
Copyright © 2026 Guts UK. This leaflet was published by Guts UK in 2021 and will be reviewed in 2024. The leaflet was written by Guts UK and reviewed by experts in biliary sphincter disorders and has been subject to both lay and professional review. All content in this leaflet is for information only. The information in this leaflet is not a substitute for professional medical care by a qualified doctor or other healthcare professional. We currently use AI translation tools on our website, which may not always provide perfect translations. Please check for further explanation with your doctor if the information is unclear. ALWAYS check with your doctor if you have any concerns about your health, medical condition or treatment. The publishers are not responsible or liable, directly or indirectly, for any form of damages whatsoever resulting from the use (or misuse) of information contained or implied in this leaflet. Please contact Guts UK if you believe any information in this leaflet is in error.



