Polyps in the Bowel
Download printable versionOverview
A polyp is a fleshy growth on the inside of the large bowel. Some people may develop a single polyp, while others may develop many.
Polyps are very common, especially in the Western world. They are a little more commonly found in men than women. They are unusual below the age of 40 and seem to occur most often in people over the age of 60. They affect one in four people over the age of 50 years.
What does a polyp look like?
A doctor or nurse may see polyps when they use a special camera, called a colonoscope, to look inside the large bowel. Polyps can look very different depending on the type found.
Some polyps have a stalk, and look like a mushroom, growing from the bowel lining (Fig. 1). Others are flatter and may have a broad base. (Fig.2)
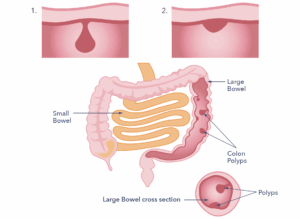
Polyps are usually benign. This means they are harmless and not cancerous. Although small polyps may be left alone, most others are usually recommended to be removed. This is because some of them may develop into cancer over time. Most experts now believe that most bowel cancers start from polyps. Doctors are most worried about a type of polyp called an adenoma polyp; these are most likely to become cancerous. It’s vital to detect these types and treat with removal when necessary. It is thought that if left alone, around 1 in 10 adenomas would develop into cancer.
Causes
The lining of the bowel, like other organ linings, constantly renews itself throughout our lives. There are many millions of tiny cells in the lining, which grow, serve their purpose and die. New cells then take their place. Each of these millions of cells contains genes, which give instructions to the cell on how to behave and grow. If genes become faulty, this can cause the cells to grow quicker. Cells that are faster growing eventually produce a small bump on the bowel surface that we call a polyp.
Some polyps remain very small (a few millimetres) while others continue to enlarge up to over 20 millimetres.
Most polyps remain harmless (non-cancerous), but it is thought that most cancers of the bowel begin as benign polyps. So, by removing benign polyps we can help to prevent the development of the rare ones that may become cancerous.
Can polyps be inherited?
Most people with polyps and cancers in the bowel do not have a genetic condition in their family. When several members of the same family have had polyps or bowel cancer there is an increased risk. The risk is higher if they have developed polyps or bowel cancer at a young age (less than 50 years old). Some of the conditions which are inherited and can cause bowel cancer are:
- Familial Adenomatous Polyposis
- Lynch Syndrome
- MUTYH associated Polyposis (MAP)
- Peutz Jeghers Syndrome (PJS)
- Juvenile Polyposis Syndrome (JPS)
- PTEN Hamartoma tumour syndrome
Tell your GP if you have a family history of the above conditions or if more than one person in your family has had bowel cancer.
Diagnosis
Bleeding from the back passage (rectal) can be a symptom of both benign and malignant polyps. It can also be a symptom of other potentially serious conditions. Investigations will find out if any of these conditions caused the bleeding.
Faecal Immunochemical test (FIT)
FIT home testing kits can pick up hidden blood in poo that is not visible to the naked eye. This test can help doctors decide if someone needs a specialist or more tests. FIT is not a direct test for polyps. It can suggest that polyps might be in the large bowel. This may lead your doctor to refer you for a colonoscopy (see below). You might be asked to do a FIT test as part of the UK bowel cancer screening programme. You will be sent a kit in the post and you need to collect a small sample of poo. The sample is then returned by post for testing. The FIT might be unpleasant to do. But, it is a small task with life-saving benefits.
Even if you have done a FIT as part of the screening programme, it is also important to check for any change in bowel habit. If you have any of the following symptoms then seek advice from your GP:
- An ongoing change in your bowel habit
- Bleeding from the bottom for no clear reason.
- Belly (abdominal) pain
- A lump in your belly
We encourage everyone who is eligible to take part in the FIT screening programme.
Everyone in England aged 54-74, who is registered with a GP, is sent a bowel screening test every 2 years. It will soon be available to people aged 50 to 74.
In Scotland and Wales, it’s everyone aged 50-74. In Northern Ireland, it’s everyone, aged 60 to 74.
If you are not registered with a GP, call the helpline:
- For England: 0800 707 60 60
- For Wales: 0800 294 3370.
- For Scotland: 0800 0121 833
- For Northern Ireland: 0800 015 2514.
If you don’t have a permanent address and live in England, ask your GP surgery to send your test kit to the surgery or another address. If you live in Wales and you are not registered with a GP contact the helpline on 0800 294 3370. The number to call in Scotland is 0800 0121 833 and Northern Ireland is 0800 015 2514.
If you live in Scotland or England and are over 75, you can request a screening kit every two years. This is done by calling the bowel cancer screening helpline on 0800 707 60 60 for England and 0800 012 1833 for Scotland
If you live in Wales or Northern Ireland there is no facility to request a test for people over 75 years of age. If you are experiencing symptoms talk to your GP.
Another time you might be asked to do a FIT test is if you go to your doctor with bowel symptoms. If the test is positive, your doctor will discuss this with you and may refer you for a colonoscopy.
Colonoscopy
A tube, linked to a highly magnified video system, is passed via the anus into the large bowel. Plus, when possible, the end part of the small bowel. A colonoscopy gives a very accurate picture of the lining of the bowel. It also allows the doctor, or nurse endoscopist, to check for polyps. The endoscopist can remove polyps during the procedure. Sometimes, a shorter camera called a sigmoidoscopy is used. The sigmoidoscopy only inspects the left side of the large bowel. If it finds a polyp, a full colonoscopy may be needed to check for more polyps in the rest of the large bowel. You can choose sedation to reduce any discomfort or anxiety.
CT Pneumocolon Scans (also known as CT virtual Colonoscopy CTVC)
This involves air being introduced into the bowel by a small tube. The air improves the views of the bowel while the scan is happening.
This test may be offered if you also are unable to complete a colonoscopy.
All of the above, except FIT, require a clear bowel before the procedure. An empty bowel is needed so that any polyps can be seen. A special diet is followed for a short time. Laxatives (medicines to make you poo) are taken at home the day before the procedure. Although unpleasant, the laxatives are taken in the right amount to clear the bowel. This will cause diarrhoea; therefore, it is a good idea to stay near a toilet.
Symptoms
Usually, polyps do not cause symptoms and most people will never know if they have them. They are usually found during a colonoscopy for another reason.
The commonest sign of a polyp will be bleeding from the back passage. This symptom doesn’t happen often. Very rarely, a polyp can grow large enough to block the bowel. But, unless this happens, polyps do not cause pain.
Will polyps in the bowel affect me over time?
Polyps rarely cause day to day problems. However, the main concern is they may become harmful and cause cancer in the future. Most polyps can be removed during your colonoscopy. However, very large polyps may need another procedure. If polyps are found and removed, they are looked at under a microscope. If cancer is found in the polyp, further tests, like scans, will be needed.
If the polyps do not contain cancer, you will be told either that nothing else is needed or that you should have another colonoscopy in a few years to monitor things. This depends on the number of polyps found and whether they were low or high-risk types. The National Institute of Health and Care excellence have guidelines for people with polyps.. See the support section for more information. Surveillance is done with a repeat colonoscopy.
You should still complete the FIT test every 2 years, if eligible, as things can change. If you have a family history of polyps or bowel cancer, your doctor may recommend regular colonoscopies.
The risk of a colonoscopy is small. But, for some, it might outweigh the benefits of screening. Discuss this with your doctor.
Diet
You do not need a special diet and can eat normally. A healthy diet is good for your overall health. It should include a variety of foods and plenty of fruit and vegetables. It will help you have regular bowel movements. Eat fruit and vegetables with meals and snacks and wholemeal or wholegrain carbohydrates with meals. Drink at least two litres (8-10 cups) of fluid daily. If you eat more than 90g of red meat per day reduce your intake to less than 70g per day. Avoid eating processed meat where possible as it carries a greater risk of developing bowel cancer. 13 out of 100 bowel cancers diagnosed are caused by eating processed meat. Red meat includes lamb, beef, pork, mutton, veal, venison and goat. Processed red meat includes sausages, bacon, ham, salami and other cured, smoked or salted meat products, canned meat and pâté. Please see our information on Healthy Eating here.
Treatment
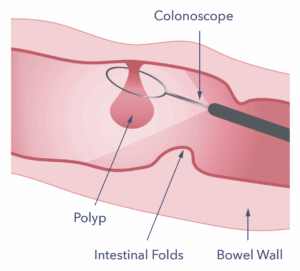
Many techniques can remove polyps. Most consist of passing a snare through the colonoscope. This consists of a wire in a loop which can be placed around the polyp, like a lasso, to remove it by cutting. This procedure is painless. Usually, one exam is enough to clear the bowel of polyps. Every once in a while, there may be too many polyps for all of them to be removed safely at once. In these cases, the procedure may need to be repeated.
If possible, the polyps are sucked up through the colonoscope after removal. They can then be sent to the laboratory to be looked at under a microscope. This will check if the polyp was fully removed. It will also look for any pre-cancerous changes and check for cancer.
Support
What to ask your doctor?
- What type of polyp do I have, is it benign or malignant?
- How often, if needed should I have a follow up colonoscopy?
- Has my family history been noted and taken into account?
- What other follow up do I need?
Where can I get more information about treatment?
The National Institute of Health and Care Excellence (NICE) produce guidelines for people with polyps. It can be found on their website here.
You can find out more about FIT testing on the NHS website here.
Research
Guts UK is proud to fund research by Professor Colin Rees. The Colorectal Cancer Cohort Study (COLO-COHORT) aims to create a better screening programme for those at high risk of bowel cancer. When identified early, Bowel cancer, is more easily and successfully treated. This Guts UK-funded research can save lives. It aims to develop a robust bowel cancer screening programme for the UK.
Copyright © 2026 Guts UK. This leaflet was published by Guts UK in August 2025 and will be reviewed in August 2027. The leaflet was written by Guts UK and reviewed by experts in polyps and has been subject to both lay and professional review. All content in this leaflet is for information only. The information in this leaflet is not a substitute for professional medical care by a qualified doctor or other healthcare professional. We currently use AI translation tools on our website, which may not always provide perfect translations. Please check for further explanation with your doctor if the information is unclear. ALWAYS check with your doctor if you have any concerns about your health, medical condition or treatment. The publishers are not responsible or liable, directly or indirectly, for any form of damages whatsoever resulting from the use (or misuse) of information contained or implied in this leaflet. Please contact Guts UK if you believe any information in this leaflet is in error.

