Rishi’s Story
Rishi is an orthopaedic surgeon and during COVID, he developed a severe abdominal pain. This is Rishi's pancreatitis story.
 My name is Rishi, I’m 40 years old and I’d say I’m someone who loves to life to the fullest – with interests in adventure sports and singing. In 2019 I started as a consultant orthopaedic surgeon and I do a lot of medical teaching too. Travelling, meeting new people and seeing my friends and family are all things I love doing.
My name is Rishi, I’m 40 years old and I’d say I’m someone who loves to life to the fullest – with interests in adventure sports and singing. In 2019 I started as a consultant orthopaedic surgeon and I do a lot of medical teaching too. Travelling, meeting new people and seeing my friends and family are all things I love doing.
I was diagnosed with gallstones aged 32, but as I wasn’t suffering from many symptoms, I chose not to have a gallbladder operation. I was at a turning point in my career so was hesitant to take time off work.
One day, results from my routine bloods returned and my GP rang to say they were concerned with the results. But again life was busy, so I organised repeat bloods to be taken and asked the place I worked at to book an ultrasound for my abdomen.
Before I could have the ultrasound, one afternoon in October I was teaching an online lesson and I started getting really bad abdominal pain that took my breath away. I tried to make it through the lesson but couldn’t concentrate. I excused myself and tried going to the toilet, but I ended up on the floor within minutes in agony and vomiting profusely. I was there for hours, trying to manage with painkillers until I rang a friend who is a consultant. He said, “it’s either a perforated organ, or you have pancreatitis”.
 I rang 111 who were asking what felt like several unrelated questions and being obstructive. Since an ambulance didn’t come, I tried to drive myself to hospital. I made it a few steps to the carpark and collapsed. I called myself a taxi to the hospital I worked at, where I called ahead. The whole journey I was vomiting bile every five minutes out of the window.
I rang 111 who were asking what felt like several unrelated questions and being obstructive. Since an ambulance didn’t come, I tried to drive myself to hospital. I made it a few steps to the carpark and collapsed. I called myself a taxi to the hospital I worked at, where I called ahead. The whole journey I was vomiting bile every five minutes out of the window.
Once there, I was given painkillers and admitted. The enzyme levels in my blood were sky high and I was diagnosed with pancreatitis caused by gallstones. I prepared myself to be off work for a couple of weeks, for a gallbladder operation and maybe a couple of other procedures for which I was transferred to another hospital. I never thought in my wildest nightmares it would be longer than this.
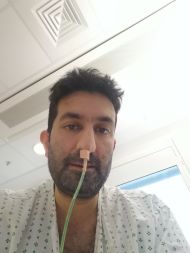 Things got worse. The acute pancreatitis became severe acute pancreatitis. My pancreas was necrotising (the tissue was dying). I was septic for six weeks and in and out of delirium. I had hallucinations where I’d see ‘evil monkeys from an Indiana Jones film’ on the drip stand. I’d hear people talking to me, or feel them touching me. I was in a very dark place with very dark thoughts. My organs began failing and as a medic, I knew exactly what was happening to me. I was dying and it was terrifying.
Things got worse. The acute pancreatitis became severe acute pancreatitis. My pancreas was necrotising (the tissue was dying). I was septic for six weeks and in and out of delirium. I had hallucinations where I’d see ‘evil monkeys from an Indiana Jones film’ on the drip stand. I’d hear people talking to me, or feel them touching me. I was in a very dark place with very dark thoughts. My organs began failing and as a medic, I knew exactly what was happening to me. I was dying and it was terrifying.
The care I experienced was variable. Some people at the hospital were incredibly helpful and communicated well with my family and I, but others would tell me, “you’ll be out in no time” or misinform me. This false sense of hope meant that every time I was told I couldn’t leave for another few weeks, it felt like I had failed. My body had failed me, where it never had before. I found the loss of control so disarming.
Facetime helped me. I spoke to family and friends, and even people I hadn’t spoken to in years. I really appreciated people stepping in to help, because I was allowed very few visitors due to COVID and it was incredibly lonely. At this point, I’d lost 3 stone in weight and couldn’t bare to look at myself in the mirror, as I felt skeletal and emasculated.
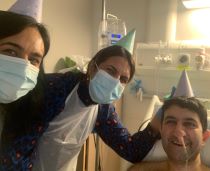 Between the end of December and March, I was in and out of hospital with various complications and having operations to drain the dead pancreas every two weeks. Every time I was admitted again, I was completely terrified. When I was home, it meant everything to be with my family. My sisters were essentially nursing me – nothing was too much trouble for them. They put their lives on hold. Even in hospital, they decorated the room as a surprise for my 40th birthday or on Christmas day. They kept me alive.
Between the end of December and March, I was in and out of hospital with various complications and having operations to drain the dead pancreas every two weeks. Every time I was admitted again, I was completely terrified. When I was home, it meant everything to be with my family. My sisters were essentially nursing me – nothing was too much trouble for them. They put their lives on hold. Even in hospital, they decorated the room as a surprise for my 40th birthday or on Christmas day. They kept me alive.
In April, I decided to have my gallbladder removed privately, as I knew that interviews for my dream job would begin in June. In hindsight, I should’ve recovered and put my career on hold, but my whole life had been on hold for months. I needed something to strive towards.
As I write this, I can tell you I got the job and I am recovering, but I’m a different person. Because I jumped back into life, I didn’t give myself time to process everything. I really underestimated the mental toll of pancreatitis. I’ll be walking down a corridor at work and I’ll get sudden anxiety. The way I handle stress is different to before. Before, I was in survival mode, but now I need to put myself into recovery mode. Above all it taught me the importance of being a  survivor and learning to live everyday as if it is my last.
survivor and learning to live everyday as if it is my last.
I contacted Guts UK about creating a big fundraising event, to give me focus and purpose through my pain. This is my way of helping others (patients and families going through suffering) and I find it therapeutic to talk to people about my experience.
"Whenever I was well enough, I spent time researching pancreatitis online. I was reading papers and mortality statistics. I was shocked at the lack of research and data surrounding pancreatitis." - Rishi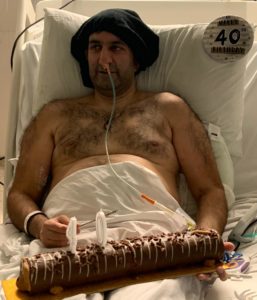 There is no effective treatment for pancreatitis. There is no cure.
There is no effective treatment for pancreatitis. There is no cure.
Guts UK is the only UK charity funding a research fellowship into pancreatitis. We are dedicated to finding an effective treatment, a cure for this misunderstood and underfunded condition.
People are suffering, people are dying, all because of a lack of knowledge about our guts. Join our community and champion our cause by donating to our life-saving research today.





