Mark’s Story
Mark had a routine gallbladder removal operation due to gallstones. The operation went well, but a week later he suffered from excruciating stomach pain. This is Mark's pancreatitis story, told by himself and his wife, Julie.
Mark:
 “I considered myself to be reasonably strong and healthy (although slightly overweight), but I enjoyed socialising and loved food. I tend to be known as the joker amongst family and friends! Work has always been my main interest, where friendships would come from as a shared bond or interest. I even met Julie, my wife at work. Then there was football with F1 as a conversation back up and interest. I just enjoyed a good conversation about anything with anyone.
“I considered myself to be reasonably strong and healthy (although slightly overweight), but I enjoyed socialising and loved food. I tend to be known as the joker amongst family and friends! Work has always been my main interest, where friendships would come from as a shared bond or interest. I even met Julie, my wife at work. Then there was football with F1 as a conversation back up and interest. I just enjoyed a good conversation about anything with anyone.
Then in July 2020, I had a routine gallbladder removal operation due to gallstones. The operation went well, but a week later I suffered from excruciating stomach pain. I went to my local walk-in centre, who advised me to go to the nearest A&E. At A&E, I was admitted with jaundice and abnormal blood test results. I was informed they suspected I had pancreatitis.
I remained in hospital. Six days on, I had a scan showing a gallstone blocking the bile duct, which they removed and fitted a stent. I was then discharged home, still in pain, in a lucid state with the painkillers and struggling to eat properly.
After two weeks of not eating properly, Julie took me back to the walk-in centre and they admitted me to a different hospital. I was put on fluids and after having a CT scan, I was told I had a large pseudocyst and severe necrotising pancreatitis. The pseudocyst was that large that it had to be drained. When draining the pseudocyst, I had to be admitted to ICU due to sepsis following complications from the procedure. I spent the next 10 days in intensive care. My wife received a phone call to come in and see me as my organs began to fail. At this point I had no idea what was going on.”
Julie:
 “When I got to the hospital, I was seen by the ICU doctor who told me they might have to put Mark onto a ventilator to drain the fluid from his body. I was told it was ‘touch and go’ whether he would survive, as his body was shutting down. Pancreatitis can affect every single organ in your body.
“When I got to the hospital, I was seen by the ICU doctor who told me they might have to put Mark onto a ventilator to drain the fluid from his body. I was told it was ‘touch and go’ whether he would survive, as his body was shutting down. Pancreatitis can affect every single organ in your body.
Later that day, I received a phone call saying they had managed to drain 5 litres of fluid from his abdomen. A few days later he was transferred onto a ward, but his lungs then started filling with fluid and he was readmitted to intensive care. I then received another phone call asking if I would consent to draining fluid from Mark’s lungs, as Mark was incapable of making any decisions. I agreed. They drained 3 litres of fluid from his lungs.
I thought we had turned a corner, but Mark couldn’t eat so he was being fed through a tube. He was tolerating this very well. At this point I was finally allowed to visit. Seeing Mark was an awful shock. He had lost 7.5 stone in weight, had complete muscle wastage and was bedridden. He weighed just 8 stone.
The doctor told me that Mark had 3 cysts on his pancreas and a lot of fluid. They needed the cysts to solidify before they could wash the infected fluid out.
Whilst on the feeding tube Mark vomited, choked and ended up back in ITU because they thought vomit had gone into his lungs. Three days later he was back out of intensive care and onto the ward. From here on, he turned the corner.
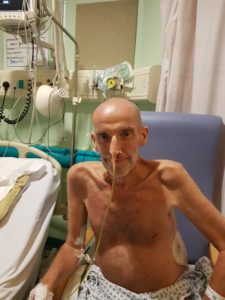 Physiotherapists were getting him out of bed every day and they put him on a different feeding tube for two weeks. After 14 weeks in hospital, thanks to the HPB team and the hospital staff, Mark was allowed to come home.
Physiotherapists were getting him out of bed every day and they put him on a different feeding tube for two weeks. After 14 weeks in hospital, thanks to the HPB team and the hospital staff, Mark was allowed to come home.
On December 21st weighing 8.5 stone and still on strong antibiotics, Mark came home. I was trained on how to administer his antibiotics, as they were done intravenously. A month later, he would stop taking the antibiotics. Then it was a slow uphill battle with eating and getting used to taking pancreatic enzymes. But gradually, Mark has gained weight and is now up to 10 stone.”
Mark:
“The professor summed up my state by saying my internal organs had the equivalent of third-degree burns. I made it through, but my struggles are ongoing. Routine blood tests showed abnormal liver results, which have resulted in jaudince and being re-admitted to hospital. There have been additional difficulities with stents that were fitted, and a potentially 5-hour-long operation to remove this stent. This is planned for next year.
Thanks to the hospital staff and the HPB department, I’m still here to share my experience. Pancreatitis is a catastrophic illness which causes upset, confusion, pain and death. This is why Guts UK needs more support, to help fight the ongoing struggles people like myself and Julie are having. If our story helps one  person or family in any way, this would make telling our story worth the while.
person or family in any way, this would make telling our story worth the while.
On a personal note, I would like to thank all the professionals, my friends and family who helped us. Most of all, my wife, who without her strength and tenacity, I feel I would have not had the same outcome. Julie gave me the strength I needed when times were looking desperate.”
"Pancreatitis is a catastrophic illness which causes upset, confusion, pain and death. This is why Guts UK needs more support, to help fight the ongoing struggles people like myself and Julie are having." - Mark There is no effective treatment for pancreatitis. There is no cure.
There is no effective treatment for pancreatitis. There is no cure.
Guts UK is the only UK charity funding a research fellowship into pancreatitis. We are dedicated to finding an effective treatment, a cure for this misunderstood and underfunded condition.
People are suffering, people are dying, all because of a lack of knowledge about our guts. Join our community and champion our cause by donating to our life-saving research today.




