Jude’s Story
Jude was diagnosed with pancreatitis before his 1st birthday. This is Jude's story as told by his mum, Nicola.
 During pregnancy with Jude, I was quite big – but so was Jude when he was born! Just four hours after he was born, my husband Dave and I took Jude home to meet his four-year-old brother, Finn. Jude was a healthy, sleepy and very chilled-out baby.
During pregnancy with Jude, I was quite big – but so was Jude when he was born! Just four hours after he was born, my husband Dave and I took Jude home to meet his four-year-old brother, Finn. Jude was a healthy, sleepy and very chilled-out baby.
We started weaning Jude at five months old. He loved trying different foods. But we soon noticed that his abdomen appeared swollen and almost solid. He wouldn’t roll on his front. I remember sending photos of his stomach to friends, asking if it looked normal to them. He started refusing milk and vomited a few times. One evening, he was desperately screaming and his abdomen looked huge. I drove him to A&E, where they discovered his abdomen was filled with fluid. We were transferred to our regional hospital and ended up staying there for 26 days, on high dependency and intensive care wards.
Many tests and scans were carried out for conditions like bowel malrotation and cystic fibrosis, but all returned negative. Jude’s fluid was drained and a scan showed a bloot clot near his liver, which they thought caused the fluid build-up. Jude was discharged with blood thinners.
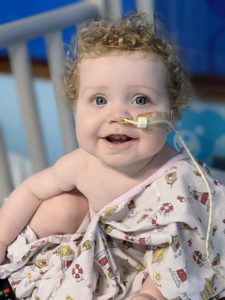 We started having frequent appointments at hospital to check Jude’s blood levels, so he got to know the staff really well. Even at six months old, Jude was a people person. He really loves going to hospital and making friends. He’d see the same person who just inserted a cannula five minutes later and would be waving and smiling at them!
We started having frequent appointments at hospital to check Jude’s blood levels, so he got to know the staff really well. Even at six months old, Jude was a people person. He really loves going to hospital and making friends. He’d see the same person who just inserted a cannula five minutes later and would be waving and smiling at them!
A month later, Jude had visible fluid build-up again. This was confirmed by ultrasound. However, the ultrasound also showed that the clot was shrinking, which suggested that the fluid build-up could be due to something else.
A few weeks on, I called our local hospital because Jude had vomited, had a low-grade fever and suddenly looked grey. Within 20 minutes of arrival he was intubated (given air via a tube). After transfer to our regional hospital ICU, Jude was diagnosed with severe sepsis, probably from the fluid which was now dangerously difficult to drain.
Jude was transferred to a high dependency unit. This began an incredibly worrying three weeks. Jude had sepsis twice more. He was nearly transferred back to ICU. There were too many scans, blood tests, investigations and blood transfusions to count. This time, Jude wouldn’t laugh or smile, which was frightening. He was in so much pain that he’d cover his eyes with his hands, almost as if he didn’t want to let people in. Jude received outstanding care from wonderful doctors and nurses who were so compassionate, dedicated and skilled. They always supported us, his parents and we cannot thank them enough.
After 10 days, the cause was finally established: pancreatitis. We were relieved that the cause had been narrowed down but it was soon explained that pancreatitis meant more months spent in hospital. Dave and I were also surprised, as Jude hadn’t been in any obvious pain when the consultants had touched his abdomen. All Jude’s blood and enzyme results had previously been normal, too.
 The cause of the pancreatitis is still unknown, even after clear genetic and autoimmune tests. There was a tear in the main pancreatic duct that might explain the pancreatitis. Some consultants said the pancreatitis could’ve been caused by an emergency brake on the motorway when he was a couple of months old.
The cause of the pancreatitis is still unknown, even after clear genetic and autoimmune tests. There was a tear in the main pancreatic duct that might explain the pancreatitis. Some consultants said the pancreatitis could’ve been caused by an emergency brake on the motorway when he was a couple of months old.
More fluid needed to be to be drained, as several cysts had extended from the tear in the pancreas. The largest was even compressing his stomach. Jude was in intense pain throughout this and needed strong painkillers. I asked the consultant if it was normal that Jude should need so much morphine for weeks due to this cyst. He said “I feel sorry for him, this is extremely painful. None of his organs are moving or making way for this pseudocyst. They’re all compressed”. We were transferred to a London hospital, where we ended up staying for two months.
Throughout this whole time, Jude was unable to see family members, including his older brother, Finn, due to COVID.
Jude continued treatment for the complications that had been caused by pancreatitis. At this point, he was so dreadfully malnourished. Jude weighed more in January at 4 months old than he did in July, at 10 months old! This meant he had a number of feeding tubes, which involved a lot of trial and error. It was a time full of uncertainity.
After three months in total, Jude was transferred back to our regional hospital for a period of weight gain before finally being discharged.
Jude gained weight well and was back to his funny, friendly and assertive little self! We were very grateful to have day release for his 1st birthday, and to have full discharge after a four month admission. He is such a little warrior, and doing well back at home with his family and his big brother. Pancreatitis is so rare in children, but can have life threatening complications.
 Jude is still having pancreatic enzymes when he eats, but we don’t know whether this is for life or not. If Jude has any future flares, he’ll have to be given blood thinners because of the way his body produced a huge blood clot during his first attack.
Jude is still having pancreatic enzymes when he eats, but we don’t know whether this is for life or not. If Jude has any future flares, he’ll have to be given blood thinners because of the way his body produced a huge blood clot during his first attack.
At present, consultants are unable to tell us whether this is something that will affect his life forever or whether it’ll never bother him again. What we do know though, is that Jude is doing far better than we ever could’ve expected just three months ago.
"Pancreatitis is so rare in children, but can have life threatening complications. That's why we so need Guts UK to carry out their research into diagnosis and treatment options for this awful condition." - Nicola, Jude's mum

There is no effective treatment for pancreatitis. There is no cure.
Guts UK is the only UK charity funding a research fellowship into pancreatitis.
People are suffering, people are dying, all because of a lack of knowledge about our guts. Join our community and champion our cause by donating to our life-saving research today.




