Henry’s Story
 Hi. My name is Henry. My pancreatitis story began when I was 11. I started to get stomach pains which were really painful. They would last around 3-4 hours and then mysteriously go away. Despite two trips to A&E, a GP appointment and 2 paramedic call-outs, my parents were told it is ‘probably indigestion’.
Hi. My name is Henry. My pancreatitis story began when I was 11. I started to get stomach pains which were really painful. They would last around 3-4 hours and then mysteriously go away. Despite two trips to A&E, a GP appointment and 2 paramedic call-outs, my parents were told it is ‘probably indigestion’.
I had several more episodes and it wasn’t until I was on holiday in Cumbria, 18 months later that we found out what was happening to me.
I started to get pains in the morning. By lunchtime, I could barely walk. I was doubled over in pain. My mum took me to the local minor injuries. There, we met a paramedic who examined me and recognised my symptoms from having seen other patients.

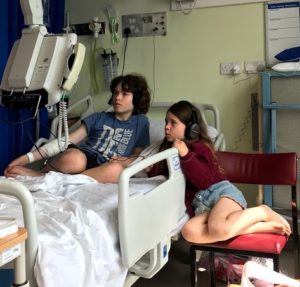
I was rushed by ambulance to hospital. Within a few hours, the blood test and ultrasound showed I had pancreatitis. I was in hospital for 5 days. My family took turns staying the night and my sister watched movies with me.
In addition to the awful pain, the most difficult part for me was having to fast and having lots of blood tests. I hate blood tests, but I have to have so many.
When we got back home, I went to see a consultant with my mum at our local hospital and was then sent to the specialist team, who I now see every 6 months. We saw a dietitian too and I was put on a low fat diet, because my pancreas is still producing enough enzymes to digest food. Though the regular pain is tough to deal with, the hardest part for me is missing school and fun trips because of pancreatitis. I also can’t eat lots of things I used to love, like pizza and chips. When I am out with friends, I have to remember to take a packed lunch and I don’t go to restaurants with my family anymore.
 I didn’t have another attack until 6 months later in February 2020. The pain was so bad. I got really angry as I couldn’t bear it. The hospital gave me morphine. Since then, I have been in hospital another 4 times. I have to have a drip to stop me getting dehydrated and lots of pain killers. When lockdown happened in March due to Covid-19, the hospital supported my parents with looking after me at home. This is so much better as I can be at home with my family, chill out in my room and spend time with my sister and friends.
I didn’t have another attack until 6 months later in February 2020. The pain was so bad. I got really angry as I couldn’t bear it. The hospital gave me morphine. Since then, I have been in hospital another 4 times. I have to have a drip to stop me getting dehydrated and lots of pain killers. When lockdown happened in March due to Covid-19, the hospital supported my parents with looking after me at home. This is so much better as I can be at home with my family, chill out in my room and spend time with my sister and friends.
I am now 13. I have attacks about every 1-2 weeks. I get really tired and have a lot of pain. I have to fast for at least 24 hours which is really hard and I get very grumpy! I keep losing weight too, which is annoying. I have missed a lot of school over the past few years, which does make me stressed having to catch up all the time. In September, I started a new school so I could be supported more. They have been brilliant. I get a lot of support from my Housemaster, teachers, school nurse and friends. The kitchen staff even make me a special meal every day so I can have lunch with everyone else.
 After my initial diagnosis, it has taken nearly a year to find out why this is happening to me. Although, I know I am lucky as some people never find out! Apparently I have the Spink I gene which means I have hereditary pancreatitis. It is strange as none of my family have ever had pancreatitis, but the gene means I am more likely to get attacks than someone without it.
After my initial diagnosis, it has taken nearly a year to find out why this is happening to me. Although, I know I am lucky as some people never find out! Apparently I have the Spink I gene which means I have hereditary pancreatitis. It is strange as none of my family have ever had pancreatitis, but the gene means I am more likely to get attacks than someone without it.
The hardest thing is not knowing when I will get an attack or what triggers them. I stick to my diet but I still get attacks and the doctors don’t seem to know how to stop them. Will this be forever? Will it get worse? I try not to think about that, as I would like to eat pizza again one day!
A word from Henry's mum, Sarah
Henry is an inspiration to me and his whole family, in how he manages his condition without complaint and just gets on with life despite the pain that he regularly suffers, the limited foods and fasting and the impact on his school and social life. I couldn’t be prouder of him.
 My experience as a parent of a child with pancreatitis has been one of frustration and often a sense of being alone in the battle. We have had to tirelessly persist at every stage, whether it was for 2 years repeatedly coming back to hospital, calling consultants and the GP to be taken seriously. Or once in receipt of a diagnosis, repeatedly insisting that we were referred to a specialist, requesting to see dietitian’s, asking for genetic tests and always quoting the NICE guidelines to anyone who would listen!
My experience as a parent of a child with pancreatitis has been one of frustration and often a sense of being alone in the battle. We have had to tirelessly persist at every stage, whether it was for 2 years repeatedly coming back to hospital, calling consultants and the GP to be taken seriously. Or once in receipt of a diagnosis, repeatedly insisting that we were referred to a specialist, requesting to see dietitian’s, asking for genetic tests and always quoting the NICE guidelines to anyone who would listen!
We are told by his consultant that there is currently no hope of a cure, or preventing these attacks and we are left with the prospect of simply monitoring his condition whilst it worsens over time, which will have a progressively negative impact on his quality of life. That for any family is a lot to take in and I want more hope than that for these kids.
If I could give one message to the medical community now, it would be to ‘Add Amylase’. If Henry had been given a simple blood test including this during his first hospital admittance, we would have been in the position to treat and attempt to prevent attacks a lot sooner. Given pancreatitis in children is relatively rare, our experience is that the majority of medical professionals do not consider it as a possible cause. I still find myself having to explain the condition and how it is treated to any new GP or medical professional that comes into contact with Henry’s case.
I would also like to see more support for families in facing the longer term implications of the disease and in our case the wider impact of genetic testing.
 Guts UK is the only UK charity funding a research fellowship into pancreatitis.
Guts UK is the only UK charity funding a research fellowship into pancreatitis.
We are dedicated to finding an effective treatment for this devastating condition. People are suffering, people are dying, all because of a lack of knowledge about our guts. Join our community and champion our cause by donating to our life-saving research today.
Be part of life-saving research. Donate to Guts UK today.