Emma’s Story
Emma's pancreatitis story, as told by her sister Chelsea as part of Guts UK's Kranky Panky Pancreatitis Awareness Campaign.
 My name is Chelsea and I want to tell my little sister Emma’s story. This is Emma’s 17-month fight with acute necrotising pancreatitis.
My name is Chelsea and I want to tell my little sister Emma’s story. This is Emma’s 17-month fight with acute necrotising pancreatitis.
Early in June 2018, Emma had been burping quite excessively. We shared a house at the time, so both went to the local chemist for help. They told Emma to take indigestion relief and make an appointment to see her GP the next day.
We came home, Emma took an indigestion tablet but 30 minutes later, I heard her shout ‘Chelsea, I think I’m dying’. She had thrown up once and it looked like coffee granules. The second time she threw up, it had blood in it. Straight away, I called 999. We thought she had a stomach ulcer that had burst.
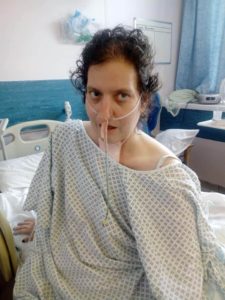 A rapid response car came with one person. While rushing to get Emma off to hospital, rapid response said to me ‘If you knew it was so serious then why didn’t you call sooner’. This has haunted me since, even though doctors have told me it was wrong, and we would never have known.
A rapid response car came with one person. While rushing to get Emma off to hospital, rapid response said to me ‘If you knew it was so serious then why didn’t you call sooner’. This has haunted me since, even though doctors have told me it was wrong, and we would never have known.
Emma was in so much pain. When we got to hospital, she explained where her pain was and was given morphine. We were told she had pancreatitis caused by gallstones and she’d likely be out of hospital in a week. A few days later, Emma started to deteriorate very rapidly. She was taken to ICU. Her organs began to fail.
In September (3 months on from entering hospital) Emma had a huge bleed where she lost 9 pints of blood. We’d been aware that the hospital had been taking Emma to theatre to ‘flush’ the pancreas, but weren’t actually told that she had necrotising pancreatitis. We later understood that they’d been flushing Emma’s pancreas because it was necrotic (dying).
This was the first (of many) times we were called and told to expect the worst. I was supporting my elderly mother and younger brother too – it was such a difficult time. We felt like the only time the hospital communicated with us was when something was very badly wrong too, when we were told to prepare for the worst.
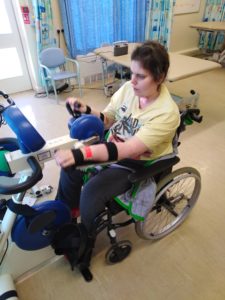 In April (10 months on from entering hospital) Emma made it to a rehabilitation centre, to learn to walk again. She spent around a month there and was doing pretty well.
In April (10 months on from entering hospital) Emma made it to a rehabilitation centre, to learn to walk again. She spent around a month there and was doing pretty well.
Unfortunately, the excess fluid in her abdomen became infected and she was transferred back to hospital. Emma’s heart was giving out, her blood pressure lowering and she just kept getting abdominal infections.
In November 2019, after a 17-month fight with pancreatitis, my sister passed away. Emma was 38 years old. She would have been 40 this November (2020).
 Emma absolutely adored animals. They were her passion; she would’ve done anything for animals. When she was well enough to speak, she would joke with the nurses at hospital, saying she loved animals more than people. During her better weeks, therapy dogs would come to see her. They would cheer her up so much.
Emma absolutely adored animals. They were her passion; she would’ve done anything for animals. When she was well enough to speak, she would joke with the nurses at hospital, saying she loved animals more than people. During her better weeks, therapy dogs would come to see her. They would cheer her up so much.
The therapy dogs even came to Emma’s funeral. We take great comfort in knowing that Emma would have absolutely loved this. Many of Emma’s nurses attended her funeral too, and we all wore purple – Emma’s favourite colour.
We didn’t know what pancreatitis was. You only briefly hear about the pancreas briefly at GCSE. I’m telling Emma’s story to get the message out there. If you have symptoms, get them looked at, push for help and even call Guts UK for advice.
Truthfully, doctors were telling us to prepare for the worst – but no one ever expected Emma to die. We would have never expected to lose a loved one to pancreatitis. If I can save one person’s life by telling Emma’s story, this can be my little sister’s legacy.
 There is no effective treatment for pancreatitis. There is no cure.
There is no effective treatment for pancreatitis. There is no cure.
Guts UK is the only UK charity funding a research fellowship into pancreatitis.
People are suffering, people are dying, all because of a lack of knowledge about our guts. Join our community and champion our cause by donating to our life-saving research today.
Chelsea shares Emma's story, as she wants her little sister's legacy to 'save lives'. When you donate to Guts UK, you fund research that has the potential to save lives.